Bone cancer on skull is a very dangerous oncological disease, because it occurs in close proximity to the brain. At the same time, in principle, this disease does not differ fundamentally from other types of bone cancer. It is advisable to treat it in a timely manner, and in this case, you can count on recovery.
Bone cancer on skull are benign or malignant neoplasms that are characteristically localized on the lower bony boundary of the brain skull, the so-called skull base. The base of the skull is the bearing surface of the brain and the dividing line to the facial skull and includes a number of openings for the passage of cranial nerves, blood vessels and the spinal cord.
The skull base can be divided into three major areas: the anterior, middle and posterior cranial fossa. Skull base tumors can occur in all three areas. Although many tumors are benign (eg meningiomas), their growth can invade healthy brain tissue, cranial nerves or blood vessels, which can ultimately lead to functional impairment or failure and thus to a neurological deficit.
A bone cancer on skull is an abnormal growth in the part of the brain that meets the base of the skull. Most skull base tumors are benign (noncancerous) and do not spread to other parts of the body. But even the benign ones, which grow slowly, can cause serious damage.
Common bone cancer on skull: MENINGIOMA, NEURINOMA, SCHWANNOMA
The most common tumors of the skull base are tumors that arise from the meninges, so-called meningiomas and neurinomas / schwannomas. Tumors in the area of the pituitary gland, so-called pituitary adenomas, are another common entity. Rarer tumors are craniopharyngiomas, chordomas, chondrosarcomas, metastases or vascular malformations. In addition, tumors from the nasal and midface area can infiltrate the base of the skull (e.g. carcinomas, esthetic neuroblastomas).
MENINGIOMAS
Overall, meningiomas account for about 25% of all tumors inside the skull. Every year about 6 out of 100,000 inhabitants fall ill, women 3-4 times as often as men. Menigeomas are usually slow-growing, benign tumors that arise from the meninges. As a rule, menigeomas grow in a crowding manner and respect a border with the brain tissue or the cranial nerves. Due to the pressure on the cranial nerves, or if they are completely surrounded by tumor tissue, these can be impaired in their function or even lose their function altogether.
In the case of sphenoorbital meningioma, the tumor grows primarily within the cranial bone, but can also perforate the dura temporally or frontally and grow intradurally, or infiltrate the orbit. This then leads to an exophthalmos and the resulting double vision.
Symptoms don’t always have to appear. Menigeomas are often an incidental finding, for example as part of a medical diagnosis of a headache. The most common skull base meningiomas are:
Meningiomas of the anterior and middle cranial fossa
- Clinoid and sphenoid wing meningioma
- Planum sphenoidale – and olfactory meningioma
- Tuberculum sellae meningioma
- Sphenoorbital meningioma
- Optic sheath meningioma
Posterior fossa meningiomas
- Tentorial meningioma
- Petroclival meningioma
- Foramen jugulare and foramen magnum meningioma
NEUROMAS AND SCHWANNOMAS
Neurinomas are benign tumors that arise from the cells that line the nerve, known as Schwann cells. Therefore, the pathophysiologically correct term is schwannoma. They make up about 8% of tumors inside the skull. Neurinomas in the interior of the skull are preferably localized in the posterior fossa, in what is known as the cerebellopontine angle, and often originate from the 8th cranial nerve. Therefore, they are typically called acoustic neuromas or vestibular schwannomas.
Typical symptoms of acoustic neuroma are hearing loss, dizziness and ringing in the ears (tinitus). In the case of very large tumors, other cranial nerves can also be affected or even brainstem compression can occur.
In addition to the acoustic neuromas, other cranial nerves can also be affected, eg trigeminal neuromas with numbness or pain in the face or glossopharyngeal neuromas with swallowing disorders.
Causes of bone cancer on skull
Currently, the specific factors leading to the occurrence of bone cancer on skull have not been identified. The immediate prerequisite for the development of this disease is a change in the structure of bone tissue cells, while their division is accelerated and the body loses control of this process.
Among the reasons that generally increase the likelihood of bone cancer on skull, we can name:
- Radiation therapy that the patient has undergone in the past
- Li-Fraumeni syndrome, it is inherited and very rare
- The presence of Olier’s disease or Paget’s disease
- Retinoblastoma, as it becomes the result of a damaged gene, while this particular gene is also responsible for bone cancer
- Umbilical hernia, which the patient had since birth.
Symptoms and signs of skull cancer
Symptoms depend on the size of the bone cancer on skull – how fast it is growing and what part of the brain it affects.
Sometimes people do not experience any symptoms and the tumor may be discovered incidentally. Often though, the patient may experience a headache, vision or hearing loss, memory problems, weakness or numbness.
Diagnosis begins with a neurological exam, followed by a CT scan or MRI of the brain. Specialized tests such as PET or cerebral angiography may be required. An image-guided biopsy (sample of the abnormal growth to see if it is cancerous) may be necessary for diagnosis.
Early signs of skull cancer include:
- Redness or inflammation in the affected area
- Palpable lump
- Swelling of the corresponding zone.
It also increases the chance of a fracture as the structure of the bone is broken.
Among the symptoms of cancer of the bones of the skull, which are not directly related to the affected area, we should mention:
- Fever over 38ºС
- Weight loss, if it is not explained by other factors
- Increased sweating, especially at night.
Depending on the location of the tumor and the proximity to neighboring structures (e.g. cranial nerves), our patients experience a wide variety of symptoms. For example, tumors in the anterior cranial fossa can lead to disorders of smell or taste, as well as psychological changes. A tumor in the middle cranial fossa can cause vision or hormonal imbalances. A posterior fossa tumor can cause hearing, balance, and swallowing disorders, as well as abnormal sensations or involuntary facial twitches.
Stages of bone cancer on skull
In total, 4 main stages of bone cancer on skull are distinguished. The first signs often make it possible to determine quite accurately how far the disease has gone.
- First stage: the tumor is localized within the skull, there is no metastasis in other tissues and lymph nodes, the neoplasm class is considered as low.
- Second stage: The tumor is still within the skull, but is already of a high grade.
- Third stage: The tumor is still inside the skull, but there are several lesions.
- Fourth stage: the tumor has metastasized to other parts of the body.
When to See a Doctor
If cancer of the skull bones is suspected, it is advisable to promptly contact an oncologist. He will accurately diagnose and offer effective treatment.
Diagnosis of cancer of the bones of the skull
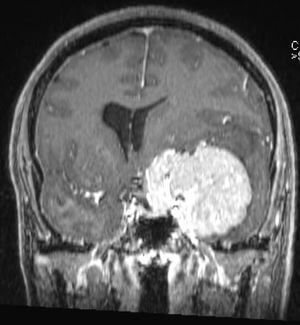
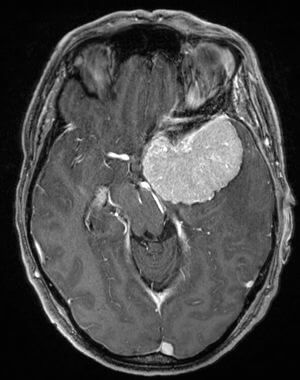
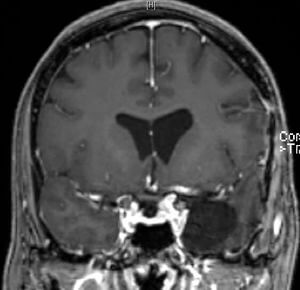
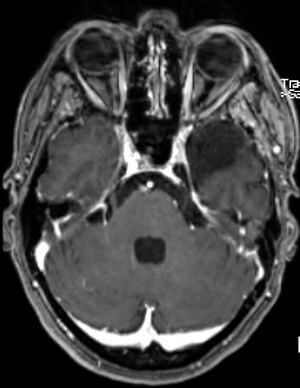
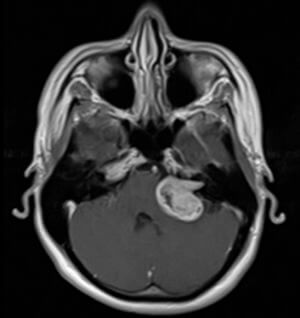
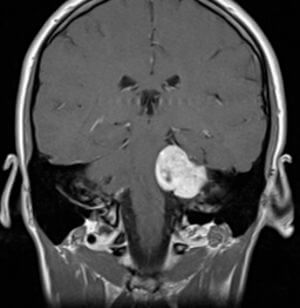
Noticed with a hearing impairment and dizziness.
There are a number of modern methods that allow you to perform the diagnosis of bone cancer on skull.
Radiography – Using X-rays, the specialist will be able to note changes in the affected skull. The area affected by cancer turns out to be “torn”, it seems that there is a hole in the skull.
Computed tomography – If bone cancer on skull is suspected, this method is more of an additional character. The reason is that this method catches other types of oncology better – neoplasms in the liver and lungs and other organs, as well as in the lymph nodes, so it is effective in stage four cancer.
Magnetic resonance imaging – This is an effective method for examining the state of the skull. It will take some time to see skull bone cancer on an MRI, as the entire procedure takes an hour.
Positron emission tomography – The patient receives some glucose solution containing radioactive atoms. This method, in combination with computed tomography, will make it possible to identify the location of tumors.
Scintigraphy or Radionuclide bone scan – Technetium bisphosphonate is a radioactive isotope, the use of which does not entail significant harm to health, is introduced into the body, after which it spreads throughout the skeleton. This is an effective way to assess the condition of the skull affected by bone cancer. In addition, using this method, it is possible to determine the degree of damage to the area affected by the disease.
Biopsy – This method consists in the direct study of bone tissue. A biopsy is performed both by making an incision on the head, and after taking samples of bone tissue for its study.
A Higher Cancer Center has all the necessary capabilities to detect bone cancer on skull and accurately assess its condition.
Treatment of bone cancer on skull
A skull affected by bone cancer can be treated with a range of modern methods.
The most radical of them are radiation therapy, chemotherapy and surgery. At the same time, there are many drugs that are used in the treatment of this disease.
Predictions of patient survival in bone cancer on skull
For an accurate prognosis, it is desirable to conduct a thorough study of skull bone cancer on MRI and other methods. According to their results, you can establish:
- Where is the primary tumor located on the skull
- Whether it has metastasized to other tissues and organs
- What is the size of the tumor.
Other factors influence the prognosis, such as:
- Whether we are talking about the very first tumor or is it a relapse
- Whether the patient had a previous cancer.
In addition, the age and gender of the applicant are important.
Prevention of cancer of the bones of the skull
Since the cause of bone cancer on skull has not been determined, experts limit themselves to standard recommendations:
- Do not drink excessive amounts of alcohol
- Stop smoking
- Do physical education
- Eat more fruits and vegetables.