Diabetes mellitus (sugar disease) is a pathological disorder of sugar metabolism. The blood sugar level of those affected is permanently elevated. Over time, this damages the blood vessels and various organs. Diabetes should therefore be recognized and treated early. Read answers to all important questions here: What exactly is diabetes? What symptoms and late effects does it cause? How do you get diabetes? How is diabetes diagnosed and treated?
Diabetes: brief overview
- Important forms: Type 1 diabetes, type 2 diabetes, gestational diabetes.
- Common symptoms: severe thirst, frequent urination, itching, dry skin, weakness, fatigue, weakened immunity.
- Possible complications: low blood sugar (hypoglycemia), high blood sugar (hyperglycemia) with hyperacidity (diabetic ketoacidosis) or extreme dehydration (hyperosmolar hyperglycaemic syndrome).
- Possible complications: retinal damage (diabetic retinopathy), kidney disease (diabetic nephropathy), diabetic foot, cardiovascular diseases, etc.
- Examinations: Measurement of blood sugar and HbA1c, oral glucose tolerance test (OGTT), test for autoantibodies (in type 1 diabetes).
- Treatment: Change in diet, regular physical activity, blood sugar-lowering tablets (oral antidiabetics), insulin therapy.
Diabetes: symptoms and consequences
The pathologically elevated blood sugar levels trigger a wide variety of symptoms in diabetes mellitus. This applies both to the two main types of diabetes (type 1 and type 2 diabetes) and to the rarer types.
Acute symptoms of diabetes occur primarily when the metabolism is derailed and the blood sugar level is extremely high. Then there are strong changes in the water and mineral balance. At the same time, there is a severe lack of energy in the body cells and in the central nervous system. The main acute diabetes symptoms are:
Increased urination
If blood sugar levels are permanently elevated, more sugar (glucose) is excreted with the urine via the kidneys (glucosuria). Since sugar physically binds water, those affected also excrete large amounts of urine (polyuria) – they have to go to the toilet very often. Many diabetics are plagued by the annoying urge to urinate, especially at night. The urine that is passed is usually clear and only slightly yellow in color.
Polyuria is a typical sign of diabetes mellitus, but can also have other causes. An increased urge to urinate also occurs with various kidney diseases and during pregnancy.
By the way: The sugar in the urine of diabetics gives it a slightly sweet taste. This is where the technical term diabetes mellitus comes from: it means “honey-sweet flow through”. However, the days when doctors still tasted their patients’ urine for diagnosis are long gone. Today, the sugar content can be detected using a rapid diabetes test with indicator sticks.
Strong thirst
The strong urge to urinate triggers a tormenting feeling of thirst in diabetic patients: the body wants to compensate for the loss of liquid by drinking more. However, this often does not succeed sufficiently. Even if those affected drink a lot, the thirst cannot really be quenched.
Weakness, tiredness and difficulty concentrating
Poor performance is also a common sign of diabetes. Because in diabetics there is a lot of energy-rich glucose in the blood. However, this cannot get into the cells to be utilized. This creates a lack of energy within the cells. As a result, patients often feel powerless and are physically less able to perform.
Most of the glucose the body needs each day is destined for the brain. A glucose deficiency therefore impairs normal brain function. It can cause poor concentration and tiredness through to severe disturbances of consciousness and coma.
Visual disturbances
If diabetes mellitus is not or not sufficiently treated, the blood sugar level is not only greatly increased, but also fluctuates greatly. These strong fluctuations can cause the lens in the eye to swell. This changes their optical refractive power and thus their visual acuity – the patients get visual disturbances. These usually last for a few hours and then subside again.
itching (pruritus) and dry skin
Sometimes diabetes causes itching and very dry skin. One reason for this is the high fluid loss as a result of increased urination (glucosuria). However, other mechanisms are also suspected that may be responsible for increased itching in diabetics. These could be, for example, stress hormones such as adrenaline and cortisol, which are increasingly released into the blood by the adrenal glands when blood sugar is too high or too low. Changes in the blood vessel walls may also contribute to the development of itching in diabetics.
Weakened immune system
The increased blood sugar weakens the immune system against infections in a way that is not yet fully understood. This is why diabetics suffer more often and longer than non-diabetics, for example from bronchitis, pneumonia, skin inflammation or various fungal diseases. The flu vaccination and the pneumococcus vaccination (pneumococci trigger pneumonia and meningitis, for example) are recommended as protection for diabetes patients.
Long-term diabetes symptoms
Late symptoms of diabetes mellitus mainly occur when the blood sugar levels are not well controlled and are often too high or unnoticed. Then blood vessels and nerves are irreversibly damaged – with serious consequences for various organ systems and bodily functions.
Nerve damage (polyneuropathy)
High blood sugar levels damage the peripheral nervous system over time. Motor (controlling the muscles) as well as sensory (feeling) and vegetative (controlling the organs) nerve tracts are affected. Diabetics therefore often have a disturbed perception of pain. For example, they do not perceive skin injuries or a heart attack as pain. Muscle coordination during movements can also suffer.
The functioning of internal organs (e.g. the digestive tract) can also be disrupted in diabetes: diarrhea and other digestive problems can result. If the high blood sugar levels damage the autonomic nervous system that supplies the digestive tract, nerve paralysis of the stomach (gastroparesis) or intestines can occur. Possible consequences are a feeling of fullness and vomiting, flatulence, diarrhea or constipation.
Damage to the blood vessels (angiopathies)
High blood sugar levels usually first trigger changes in the inner wall layer of the small and smallest blood vessels (capillaries) (microangiopathy). Over time, the medium and large blood vessels can also become damaged (macroangiopathy). The vascular damage results in circulatory disorders up to complete closure. A wide variety of organs can be affected. Here are the most important examples:
- Heart : The narrowing or blockage of small blood vessels reduces the supply of oxygen to the heart muscle. Possible consequences are cardiac insufficiency, coronary artery disease and myocardial infarction.
- Brain: Circulatory disorders in the brain impair brain performance and can trigger chronic neurological deficits. In the worst case, a stroke occurs.
- Eyes: Damage to the blood vessels in the retina of the eye (diabetic retinopathy) causes symptoms such as ” flashes of light “, blurring of vision, impaired color vision and eventually loss of vision to the point of blindness.
- Kidneys: Here, circulatory disorders cause changes and damage to the tissue. This diabetic nephropathy can eventually lead to impaired kidney function (renal insufficiency). If the kidneys fail completely, the patients are dependent on blood washing (dialysis) in the long term.
- Skin: Due to damage to the small skin vessels, the skin is more susceptible to colonization with germs (skin infections). In addition, poor wound healing is observed. Poorly healing chronic wounds and ulcers in the lower leg/foot area are called diabetic foot.
Diabetes and depression
About a quarter of all diabetes patients suffer from a depressed mood or depression. The trigger is usually the diabetes itself as well as possible long-term effects that can put a great deal of psychological strain on those affected.
Conversely, people with depression also have an increased risk of developing type 2 diabetes. One reason for this could be that depressed people pay less attention to a healthy lifestyle, for example, eat unhealthily and exercise little. Such factors contribute to the development of type 2 diabetes. In addition, depression could change the patient’s hormonal system and metabolism via various signaling pathways in such a way that diabetes is promoted.
Regardless of the exact connection between diabetes and depression, both diseases should be treated professionally. Otherwise, the patient’s health may deteriorate. For example, many depressed patients neglect blood-sugar-lowering therapy – they no longer take blood-sugar tablets or insulin injections very seriously.
To treat depression, the doctor only prescribes certain active ingredients for diabetics. Some medications have a negative effect on weight and blood sugar. For example, the selective serotonin reuptake inhibitors (SSRI) that are customary anyway, such as sertraline, are suitable. With the right therapy, not only the depressive moods improve. It can also result in better blood sugar levels.
Diabetes and impotence
Many male diabetics complain of erectile dysfunction. The reason: the high blood sugar levels damage the blood vessels in the cavernous bodies of the penis. This can affect the blood flow needed for an erection. Damage to the autonomic nervous system, which is important for erection, and the sensory nerve tracts can also play a role in the development of impotence in diabetes mellitus.
Causes and risk factors of diabetes mellitus
All forms of diabetes mellitus are based on impaired blood sugar regulation. You can only understand more precisely if you know the basics of blood sugar regulation:
After a meal, the food components such as sugar (glucose) are absorbed into the blood via the small intestine, which causes the blood sugar level to rise. This stimulates certain cells in the pancreas – the so-called “Langerhans beta islet cells” (beta cells for short) – to release insulin. This hormone ensures that the glucose gets from the blood into the body cells, where it serves as an energy supplier for the metabolism. Insulin lowers the sugar level in the blood.
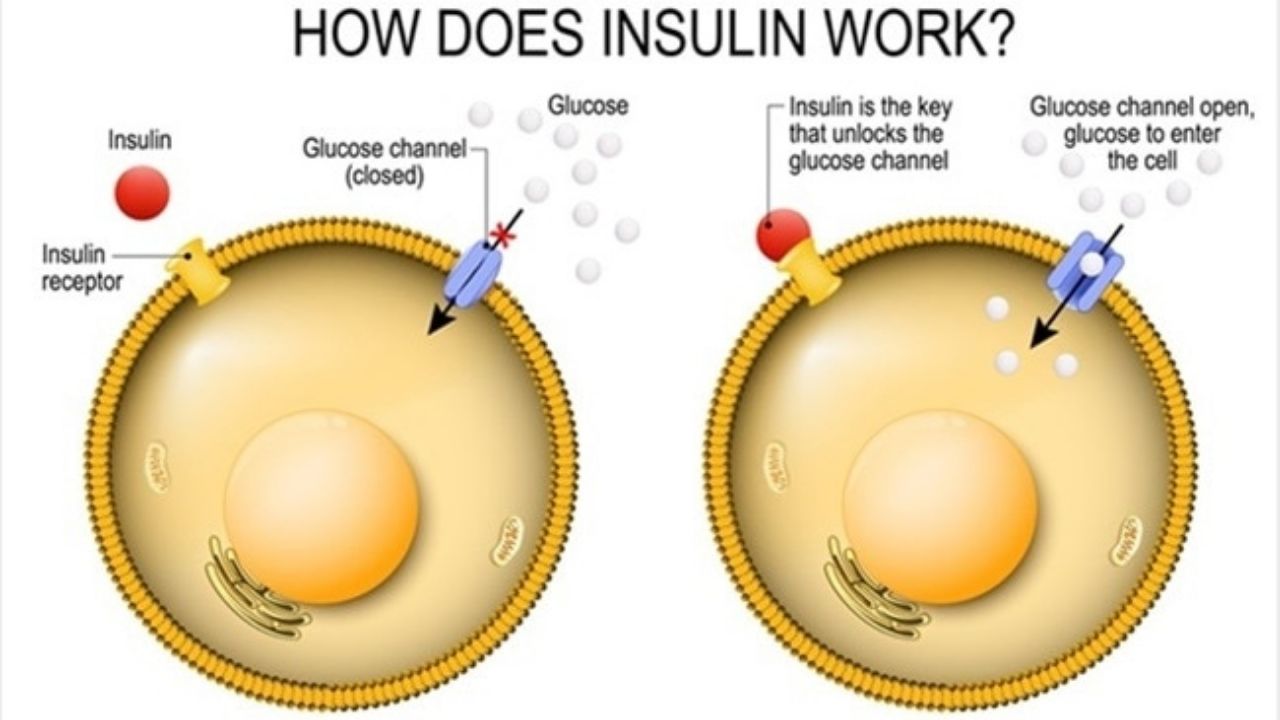
This causes the channel for the uptake of sugar (glucose) into the cell to open, allowing sugar from the blood to enter the cell.
In the case of diabetes, this blood sugar regulation is disturbed at (at least) one important point.
Type 1 diabetes mellitus
In type1 diabetes mellitus, the site of the disturbed blood sugar regulation is the pancreas: the insulin-producing beta cells in the patient are destroyed by the body’s own antibodies. These autoantibodies mistake the beta cells for dangerous or foreign and attack them. Children with type 1 diabetes in particular often also have autoantibodies against insulin.
Type 1 diabetes is an autoimmune disease. It is not yet known exactly why it occurs. Experts assume a genetic predisposition and various risk factors (such as infections) that favor the development of this diabetes.
The destruction of the beta cells results in an absolute lack of insulin. People with type 1 diabetes have to inject insulin throughout their lives to compensate.
Type 2 diabetes mellitus
In type 2 diabetes, the starting point of the disturbed blood sugar regulation is in the body cells: the pancreas usually produces enough insulin at the beginning. However, the body cells are becoming increasingly insensitive to it. This insulin resistance triggers a relative lack of insulin: Actually, there would be enough insulin, but it can only unfold its effect insufficiently. In response, the body causes the beta cells to make more and more insulin. The pancreas cannot keep up this overproduction forever: Over time, the beta cells become exhausted, so that insulin production decreases. Then there is an absolute lack of insulin.
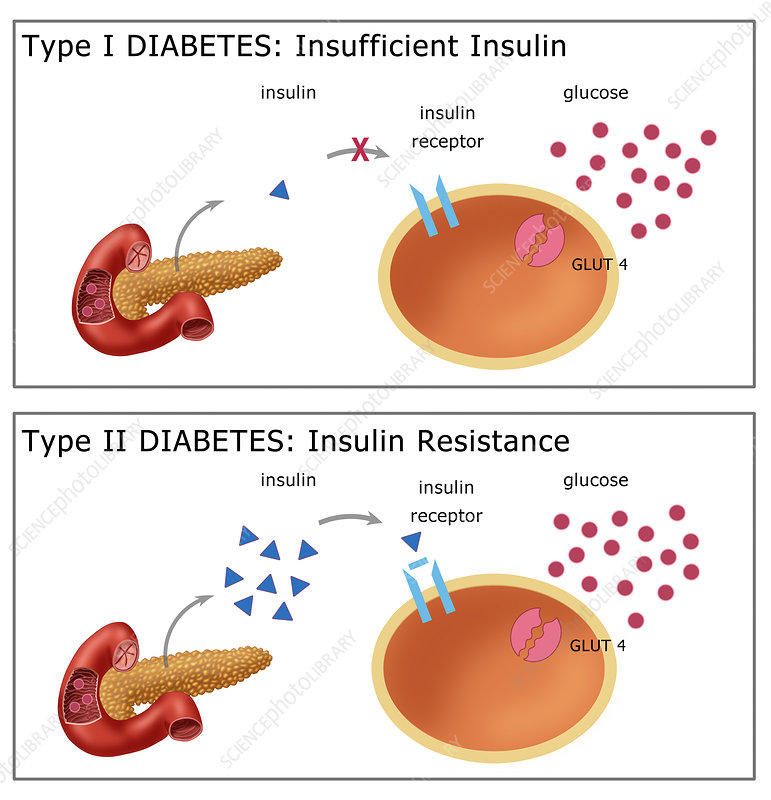
In both cases, the sugar can no longer be absorbed into the body cells and the sugar level in the blood rises.
It is not known exactly why some people develop these pathologies and thus type 2 diabetes. However, unfavorable lifestyle factors play a major role:
Most type 2 diabetics are overweight or even obese. The fat cells in the abdominal area in particular produce inflammatory substances that can cause insulin resistance. An increased abdominal circumference therefore increases the risk of type 2 diabetes mellitus. The same applies to other factors such as smoking and lack of exercise. A genetic component is also attributed to type2 diabetes mellitus.
Gestational diabetes
Some women become temporarily diabetic during pregnancy. Doctors then speak of gestational diabetes (or type 4 diabetes). Various factors appear to be involved in its formation:
During pregnancy, more hormones are released that are antagonists of insulin (e.g. cortisol, estrogen, progesterone, prolactin). In addition, affected women apparently have chronically reduced insulin sensitivity: the body cells therefore respond less to insulin. This gets worse as the pregnancy progresses.
In addition, there are some factors that increase the risk of gestational diabetes. These include, for example, obesity and diabetes in the family.
Type 3 diabetes mellitus
There are some rare type of diabetes, sometimes grouped together under the term type 3 diabetes. They have causes other than type 1 and type 2 diabetes and gestational diabetes.
One example is MODY (maturity onset diabetes of the young), also known as type 3a diabetes. It includes various types of diabetes that occur in children and adolescents (before the age of 25). They are caused by certain genetic defects in the beta cells of the pancreas.
In contrast, type 3b diabetes is based on genetic defects that impair insulin action. If certain chemicals or medications are the cause of diabetes, doctors speak of type 3e.
Diabetes in children
Most diabetic children have type 1 diabetes. In the meantime, however, more and more offspring are also developing type 2 diabetes:
In the past, this was mainly a problem for older people – hence the earlier term “adult-onset diabetes” for type 2. However, the modern, Western way of life has meant that more and more children and young people are showing the main risk factors for the disease. These are obesity, lack of exercise and an unhealthy diet. This is why type 2 diabetes is now becoming more common among young people.
Diagnosis of diabetes mellitus
The right contact person if you suspect diabetes is your family doctor or a specialist in internal medicine and endocrinology. However, the vast majority of all diabetes is due to type 2 diabetes – and this only develops slowly. Some symptoms (such as tiredness or visual disturbances) are not directly related to the sugar metabolism by the patients.
Many people therefore ask themselves: “How do I recognize diabetes? What are the signs that I should be aware of possible diabetes?” The answer: If you can answer “yes” to one or more of the following questions, you should talk to your doctor about it:
- Have you recently felt a tormenting feeling of thirst without any unusual physical exertion and have you been drinking significantly more than usual?
- Do they urinate frequently and in large quantities, including at night?
- Do you often feel physically weak and tired?
- Is diabetes known in your family?
Interview and physical examination
The doctor will first talk to you in detail to collect your medical history. For example, he will ask you about your symptoms. Also describe to him any complaints for which you actually suspect another cause (such as stress as the reason for concentration problems).
Also tell your doctor about any concomitant diseases such as high blood pressure or circulatory disorders in the legs. They could already turn out to be consequences of long-standing type 2 diabetes.
The interview is followed by a physical examination. Here the doctor pays attention to how well you can feel fine touches on your hands and feet. If hardly or not at all, this could already indicate diabetes-related nerve damage (diabetic polyneuropathy).
Measurement of blood sugar (diabetes tests)
Measuring blood sugar levels is understandably the most meaningful thing about diabetes. The following investigations play a special role:
- Fasting blood glucose : measurement of blood glucose after at least eight hours without food.
- HbA1c : so-called “long-term blood sugar”, also important for the course of the disease.
- Oral Glucose Tolerance Test (OGTT) : a “sugar load test” in which the patient drinks a defined sugar solution; then the blood sugar levels are measured at certain intervals.
These examinations are often summarized under the term diabetes tests. This often includes urine tests, which are carried out if diabetes is suspected. Sugar can be detected in the urine of diabetics (glucosuria) – but not in healthy people.
Doctors do blood and urine tests to diagnose diabetes. Some self-tests are also commercially available that any layman can carry out independently at home. However, they do not allow a diagnosis – if the test results are abnormal, you should go to the doctor for a more detailed examination.
diabetes values
Diabetes is present when the values for the fasting blood sugar, the HbA1c or the oral glucose tolerance test are too high. But what does “too high” mean? What thresholds mark the transitions from “healthy” to “impaired glucose tolerance” and on to “diabetes”?
The following applies to the fasting blood sugar, for example: If it is repeatedly 126 mg/dl or higher, the patient is diabetic. If repeated measurements result in values between 100 and 125 mg/dl, there is an impaired glucose tolerance. It is regarded as a precursor to diabetes (“prediabetes”).
The various diabetes values not only play a decisive role in the diagnosis of diabetes. They must also be checked regularly afterwards: This is the only way to assess the course of the disease and the effectiveness of the diabetes treatment. Some of the control measurements are carried out by the patients themselves (e.g. blood sugar measurement).
Antibody test for type 1 diabetes
The detection of antibodies against the beta cells (islet cell antibodies) or against insulin (insulin antibodies) is also helpful in diagnosing the autoimmune disease type 1 diabetes. In many of those affected, these autoantibodies can be detected in the blood long before the first symptoms appear.
An antibody test may also be indicated to distinguish between type 1 and type 2 diabetes – for example, when type 2 is unusually present at a young age.
Further investigations
Further examinations serve to identify possible consequences of diabetes at an early stage. For example, the doctor will examine whether your sense of touch in your hands and feet is normal. Elevated blood sugar levels can damage nerves. This causes sensory disturbances over time.
The vascular damage can also affect the retina of the eyes. The doctor therefore checks whether your vision has decreased. A special eye examination is then usually carried out by the ophthalmologist.
Treatment of diabetes mellitus
Therapy for diabetes mellitus aims to lower the elevated blood sugar level and prevent harmful consequences of diabetes on blood vessels, nerves and organs. On the one hand, this should be achieved through non-drug measures : Above all, the right diet and sufficient exercise can improve blood sugar levels. Regularly measuring the blood sugar level helps to keep track of the progress of the disease (possibly with the help of a diabetes diary).
On the other hand, diabetes treatment often requires additional diabetes medication (antidiabetics). Oral preparations (blood sugar-lowering tablets) and insulin, which must be injected, are available. Which antidiabetics are used in individual cases depends on the type of diabetes and the severity of the disease.
In the following you will find more information about the various measures of diabetes therapy:
Diabetes Education
If diabetes is diagnosed, patients should attend diabetes education. There they learn everything important about their illness, the possible symptoms and consequences as well as the treatment options. Diabetics also learn in the training what can lead to sudden complications (such as low blood sugar) and what to do then.
Diabetes Diary
After being diagnosed with diabetes mellitus, you need to measure your blood sugar levels regularly regularly . For a better overview you should keep a diary. All measured values are logged there. You can also enter other important parameters, such as the use and dosage of blood sugar tablets or insulin or blood pressure readings. Take the diary with you when you go to the doctor.
Such a diabetes diary is particularly advisable for type 1 diabetics with so-called “brittle diabetes”. This is an outdated term for type 1 diabetics who suffer from severely fluctuating blood sugar levels (brittle = unstable). The metabolic disorders can make numerous hospital stays necessary.
Diabetes nutrition
A varied and balanced diet is important for everyone, but especially for diabetics. It is important to avoid massive blood sugar spikes after eating and sudden hypoglycaemia. Patients should therefore immediately receive individual nutritional advice after being diagnosed with diabetes. There they learn how to eat properly and healthily.
If patients consistently implement the individual nutritional recommendations, they can make a significant contribution to lowering their blood sugar levels and keeping them under control. Therefore, an adapted diet is part of any diabetes therapy.
Bread units
A special role in the correct diet of diabetic patients play the Carbohydrates. They are mainly responsible for the increase in blood sugar levels after eating. Patients in particular who inject insulin must therefore be able to estimate the amount of carbohydrates in a planned meal. This is the only way they can choose the right dose of insulin.
In order to make it easier to assess the carbohydrate content of a food, the Bread units (BU) were introduced The following applies: 1 BU corresponds to 12 grams of carbohydrates. For example, a slice of wholemeal bread (60 grams) has 2 bread units. A glass of carrot juice provides 1 BU.
diabetes and exercise
Diabetics can benefit from physical activity in several ways:
Firstly – regular physical activity supports the reduction of excess weight, from which many type 2 diabetics suffer. Obesity is often the main reason why the body cells respond less to insulin.
Second – muscle work also directly increases the insulin sensitivity of the body’s cells. This improves the absorption of sugar from the blood into the cells. Anyone who is regularly active in sports can often reduce the dose of blood sugar-lowering medication (tablets or insulin) (only in consultation with the doctor!).
Third – physical activity improves well-being and quality of life. This is particularly important for people with chronic diseases such as diabetes. The chronic condition can be psychologically very stressful and contribute to depressive moods.
Diabetics should therefore make sure they get enough exercise in their everyday life and exercise regularly – of course adapted to their age, physical fitness and general state of health. Let your doctor or a sports therapist advise you on which and how much sport you can do and what you have to pay attention to when training.
Physical activity can greatly lower blood sugar. Diabetics must then closely monitor their blood sugar levels and practice the correct adjustment of insulin and sugar intake.
Oral diabetes medication
The basis of any type 2 diabetes treatment is a lifestyle change. This includes, above all, a change in diet as well as regular exercise and sport. Sometimes these measures are enough to lower the blood sugar levels of type 2 diabetics to a healthier level. If not, the doctor will also prescribe oral antidiabetics. In some cases, drugs that are injected under the skin are also used.
There are different substance classes of these diabetes medications in tablet form. They differ in the mechanism of action with which they lower elevated blood sugar levels. Metformin and so-called sulfonylureas (such as glibenclamide) are most commonly prescribed.
Initially, an attempt is made to get the blood sugar levels of type 2 diabetics under control with just one such oral antidiabetic (monotherapy). If this is not successful, the doctor prescribes other diabetes tablets or insulin (combination therapy). Type 2 diabetes mellitus is rarely treated exclusively with insulin (see below).
By the way: Oral antidiabetics are not normally used in type 1 diabetes – they do not achieve sufficient success here. They can only be useful in overweight patients with an increased risk of heart disease.
For the treatment of gestational diabetes In addition, they are not approved Metformin is only used in very rare exceptional cases, if absolutely necessary, in pregnant women to lower severely elevated blood sugar levels (“off-label use”).
insulin therapy
The treatment of type 1 diabetes aims to compensate for the patient’s absolute lack of insulin. This is only possible with insulin injections. This means that every type 1 diabetic has to self- administer insulin on a regular basis. Type 2 diabetics and women with gestational diabetes rarely need insulin. Insulin therapy can be done in different ways:
Conventional insulin therapy
In conventional insulin therapy, the insulin is injected according to a fixed schedule, usually in the morning and evening. Conventional insulin therapy is therefore easy to use. However, it restricts the patient: major deviations from the usual eating plan are not possible, and extensive physical activity can lead to problems. Conventional insulin therapy is therefore particularly suitable for patients who can stick to a fairly rigid daily and nutritional plan and for whom it would be too difficult to implement intensified insulin therapy.
Intensified insulin therapy (ICT diabetes)
The intensified insulin therapy attempts to imitate the physiological insulin release as precisely as possible. Accordingly, insulin administration is more difficult than with conventional insulin therapy. It is based on the basic bolus principle:
The patients inject a small amount of long-acting insulin once or twice a day to cover the basic need for insulin (basic insulin). In addition, normal insulin or short-acting insulin is injected before a meal . This bolus insulin is intended to “intercept” the expected increase in blood sugar (due to eating). Patients have to calculate its dose by taking into account the current blood sugar level, the time of day and the planned meal.
Intensified insulin therapy requires good training and very good patient cooperation (compliance). Otherwise, incorrect calculations of the insulin dose can easily lead to dangerous diabetes hypoglycaemia.
The advantage of the basic bolus concept is that, when used correctly, it allows very good blood sugar control. In addition, patients can eat whatever they want and exercise as they please.
Insulin pump (“diabetes pump”)
Diabetes treatment with an insulin pump is also called continuous subcutaneous insulin infusion therapy (CSII). The small device consists of a pump with an insulin reservoir, which the diabetic patient always carries with them (e.g. on their waistband). The pump is connected to a small needle via a thin hose, which remains permanently in the subcutaneous fatty tissue (usually on the stomach).
The programmable insulin pump regularly and automatically delivers small amounts of insulin to the tissue that cover the basal needs. The device mimics the function of the pancreas. Before a meal, the patient can set off an additional amount of insulin (bolus) at the touch of a button, adjusted to the meal, the time of day and the current blood sugar level.
The insulin pump saves type 1 diabetics from having to handle insulin syringes and allows for flexible meal planning and spontaneous sporting activities. This is particularly important for young patients. In addition, the blood sugar can be adjusted to be even more stable here than with insulin injections. Many patients report that their quality of life has improved significantly thanks to the “diabetes pump”.
The setting and adjustment of the insulin pump should be done in a specialized diabetes clinic or practice. Patients must be fully trained in the use of the pump. Dosing errors can quickly become life-threatening! In addition, the patient must immediately switch to insulin syringes if, for example, the insulin pump fails or is to be taken off for a longer period of time.
Continuous Glucose Monitoring (CGM)
A more recent development is a small glucose sensor that is inserted into the patient’s subcutaneous fatty tissue (e.g. on the abdomen). It measures the glucose content in the tissue. The measurement results can be transmitted wirelessly, for example to a small monitor to support intensified insulin therapy (sensor-assisted insulin therapy, SuT). The measured values can also be forwarded directly to an insulin pump (sensor-assisted insulin pump therapy, SuP). The CGM offers various alarm options that warn the patient when a high or low blood sugar is imminent.
However, it is important that the patients measure their blood sugar themselves, at least in certain situations , for example after exercising or before a planned dose of insulin. Because there is a natural difference between the tissue sugar (recorded by the CGM) and the blood sugar: Above all, the tissue sugar lags behind that in the blood – about five to 15 minutes, possibly a little longer. If the blood sugar already falls after physical exertion, for example, the tissue measurement may continue to show normal values.
Various insulins are used in the treatment of diabetes mellitus. Mostly it is artificially produced human insulin. In addition to human insulin, porcine insulin and insulin analogues are also available. Insulin analogues are also man-made. However, their structure differs slightly from that of human insulin and thus of human insulin.
Insulin preparations can be classified according to their onset of action and their duration of action. For example, there are short-acting and long-acting insulins. It is very important for successful diabetes treatment that the right insulins are administered at the right time and in the right dosage.
“DMP – Diabetes” (Disease Management Program)
Diabetes mellitus is one of the most common chronic diseases in western industrialized countries. So-called disease management programs are therefore becoming increasingly important. They are originally from the USA. This is a concept organized by the health insurance companies, which is intended to make it easier for treating physicians to offer a standardized, close-meshed range of therapy and care for the chronically ill. In the case of diabetes, this includes information brochures, counseling sessions and training courses on the subject of diabetes.
Diabetes: course of the disease and prognosis
The course of the disease and the prognosis are very different for the individual types of diabetes. However, patients with all forms of diabetes can positively influence the course of the disease if they conscientiously implement the therapy recommendations ( adherence to therapy = compliance). This prevents complications and significantly reduces the risk of complications from diabetes.
Regular check-ups at the doctor ‘s are also important for diabetics . For example, signs of complications from diabetes can be recognized and treated at an early stage.
Whether diabetes can be cured depends on the form of the disease. Type 1 is currently usually an irreversible diagnosis. In type 2, at least in the early stages, consistent lifestyle changes can significantly alleviate the disease. Sometimes no further therapy is necessary. As a rule, complete diabetes healing is only possible in the case of type 4 diabetes mellitus (gestational diabetes): After the hormonal state of emergency during pregnancy, the woman’s body usually returns to its normal status and the diabetes disappears.
In the case of diabetes mellitus, life expectancy depends on whether the blood sugar can be controlled well over the long term and how consistently the patient adheres to the therapy (compliance). Possible concomitant and secondary diseases such as high blood pressure, elevated blood lipid levels or kidney weakness also have a major impact. If they are treated professionally, this can have a positive effect on life expectancy.
Complications of diabetes mellitus
If diabetes mellitus is poorly controlled, there is a risk of acute metabolic disorders – either because the blood sugar is far too low (hypoglycaemia) or far too high (hyperglycaemia). In the second case, hyperosmolar hyperglycemic syndrome or diabetic ketoacidosis may occur. Both can lead to a diabetic coma (coma diabeticum).
By the way: The transitions between normal blood sugar levels, low and high blood sugar levels are fluid.
In the long run, poorly controlled blood sugar levels can trigger secondary diseases. For example, high levels of blood sugar damage the blood vessels (diabetic angiopathy), which results in circulatory disorders. This can result, for example, in “intermittent claudication” (PAD), kidney disease (diabetic nephropathy), eye disease (diabetic retinopathy), heart attack or stroke. The nerves are also damaged in diabetic patients (diabetic polyneuropathy). This leads, for example, to diabetic foot syndrome.
Below you can read more about diabetes complications and secondary diseases.
low blood sugar (hypoglycemia)
Critically low blood sugar is the most common complication in patients with diabetes. It is caused by too much insulin in the blood for current needs. Diabetes patients who inject insulin or take tablets that stimulate insulin production (sulfonylureas or glinides) are particularly at risk of hypoglycaemia:
If you accidentally overdose on your medication, your blood sugar levels will drop too low. Skipping a meal or vigorous exercise can also trigger hypoglycemia if drug therapy is not adjusted appropriately.
Patients with low blood sugar sweat, tremble and get tachycardia, among other things. Severe hypoglycaemia can be life-threatening.
Hyperosmolar Hyperglycemic Syndrome (HHS)
This severe metabolic imbalance occurs primarily in older type 2 diabetics. If they make mistakes using insulin or oral antidiabetics, insulin deficiency results. From this, an HHS slowly develops over days to weeks:
Blood sugar rises to extremely high levels (> 600 mg/dl). Due to physical laws (osmosis), the large amount of sugar withdraws large amounts of liquid from the body cells. As older patients generally tend to drink little, this can lead to extreme dehydration.
The signs of HHS develop slowly. Initially, uncharacteristic symptoms such as exhaustion and drowsiness appear. There are also other symptoms such as blurred vision, frequent urination, great thirst, leg cramps, weight loss and low blood pressure. Neurological symptoms such as speech disorders and hemiplegia are also possible. In extreme cases, disturbances of consciousness up to and including unconsciousness (coma) occur. Then there is danger to life!
The hyperosmolar hyperglycaemic syndrome must be treated immediately by a doctor! In the event of impaired consciousness, the emergency doctor must be alerted immediately!
Diabetic ketoacidosis is also the result of high blood sugar (hyperglycemia). It occurs preferentially in type 1 diabetics:
Due to the absolute insulin deficiency of those affected, not enough “fuel” for energy production (blood sugar) can get into the cells. The liver then tries to compensate for the lack of energy by producing new glucose (gluconeogenesis) and breaking down fat. However, gluconeogenesis only exacerbates hyperglycemia. And when fat is broken down, acidic metabolites (ketone bodies) are formed. The body can only exhale part of it in the form of carbon dioxide through the lungs. The rest “acidifies” the blood – acidosis develops.
The triggers are usually physical stressful situations such as an infection: the body then needs more insulin than normal. If the insulin therapy is not adjusted accordingly, there is a risk of a metabolic imbalance. The same can happen if insulin syringes are forgotten or underdosed, or the insulin pump malfunctions.
Those affected feel increased thirst, nausea and vomiting, loss of appetite, abdominal pain and severe tiredness. Particularly typical are strikingly deep breathing (kissing mouth breathing) and an acetone smell in the exhaled air (smell of apple or even nail polish remover). Left untreated, disorders of consciousness up to and including unconsciousness (coma) can occur. Then there is danger to life!
Diabetic Ketoacidosis is a Medical Emergency! Those affected must be taken to a hospital immediately and treated in the intensive care unit.
Poorly controlled blood sugar levels in diabetes damage the small blood vessels in the retina in the eyes. This is how a retinal disease develops, which is called diabetic retinopathy.
Affected patients experience visual disturbances. Your eyesight is deteriorating. In extreme cases, there is a risk of blindness. In industrialized countries, diabetic retinopathy is the leading cause of blindness in middle age and the third most common across all age groups.
If the retinal disease has not progressed too far, the course can be stopped with laser therapy.
Like diabetic retinopathy, diabetes-related kidney disease is based on damage to small blood vessels (microangiopathy) caused by poorly controlled blood sugar levels. The kidneys can then no longer adequately fulfill their functions. This includes the filtering (detoxification) of the blood and the regulation of the water balance.
Possible consequences of diabetic nephropathy are kidney-related high blood pressure, accumulation of water in the tissue (oedema), lipid metabolism disorders and anemia. Kidney function can continue to deteriorate – up to chronic kidney failure.
Diabetes with persistently poorly controlled blood sugar can damage and disrupt nerves. This diabetic polyneuropathy first appears on the foot and lower leg – a diabetic foot develops (see below).
Diabetic neuropathy can also affect other nerves in the body. For example, nerve damage in the autonomic nervous system causes low blood pressure, bladder emptying disorders, and constipation or the inability to control bowel movements. Gastric paralysis with nausea and vomiting (diabetic gastroparesis) can also occur. Some patients also suffer from tachycardia or increased sweating. Erection problems are often observed in male patients.
Diabetic foot syndrome develops on the basis of diabetes-related nerve damage and diabetes-related vascular damage:
The nerve disorders trigger abnormal sensations (such as “pins and needles”) and sensory disturbances in the foot and lower leg. The latter cause patients to perceive heat, pressure and pain (e.g. due to shoes that are too tight) only to a lesser extent. In addition, there are circulatory disorders (as a result of the vascular damage). All of this together leads to poor wound healing. This is how chronic wounds can develop, which often also become infected. Gangrene can also occur, in which case the tissue dies. In the worst case, an amputation is necessary.
severely handicapped pass
Diabetes patients can take advantage of special facilities for the severely disabled. A severe disability exists when the therapy effort is very high and the person concerned is severely restricted in everyday life due to the illness. In the meantime, many people affected apply for a disability card every year. As a result, diabetes patients receive important compensation for disadvantages such as tax breaks, free transport on public transport or reduced admission to cultural institutions.
living with diabetes
Diabetes mellitus can affect the entire life of those affected. This starts with small things (such as alcohol consumption at family celebrations) and extends to life issues such as family planning and the desire to have children.
Travel is also an important topic for many diabetics: what do I have to consider as a diabetic when traveling by plane? What medicines and medical supplies do I need to take with me? How to store them What about vaccinations?
