Endometriosis is one of the most common diseases of the female reproductive system; when it occurs, the cells of the endometrium (the layer that lines the uterus from the inside) grow outside of it.
Endometriosis is found not only in parts of the reproductive system, but also outside it (abdominal wall, urinary system, digestive tract, peritoneum, lungs, etc.). Clinical manifestations are varied and depend on the location of the pathological process. They can be expressed by: pain, menstrual irregularities (bloody discharge before the onset of menstruation, contact bleeding).
Infertility, menstrual irregularities, and polycystic ovary disease can result from genital endometriosis. According to research data, every third gynecological disease (excluding inflammatory diseases and fibroids) in a woman is endometriosis or a pathological process caused by it.
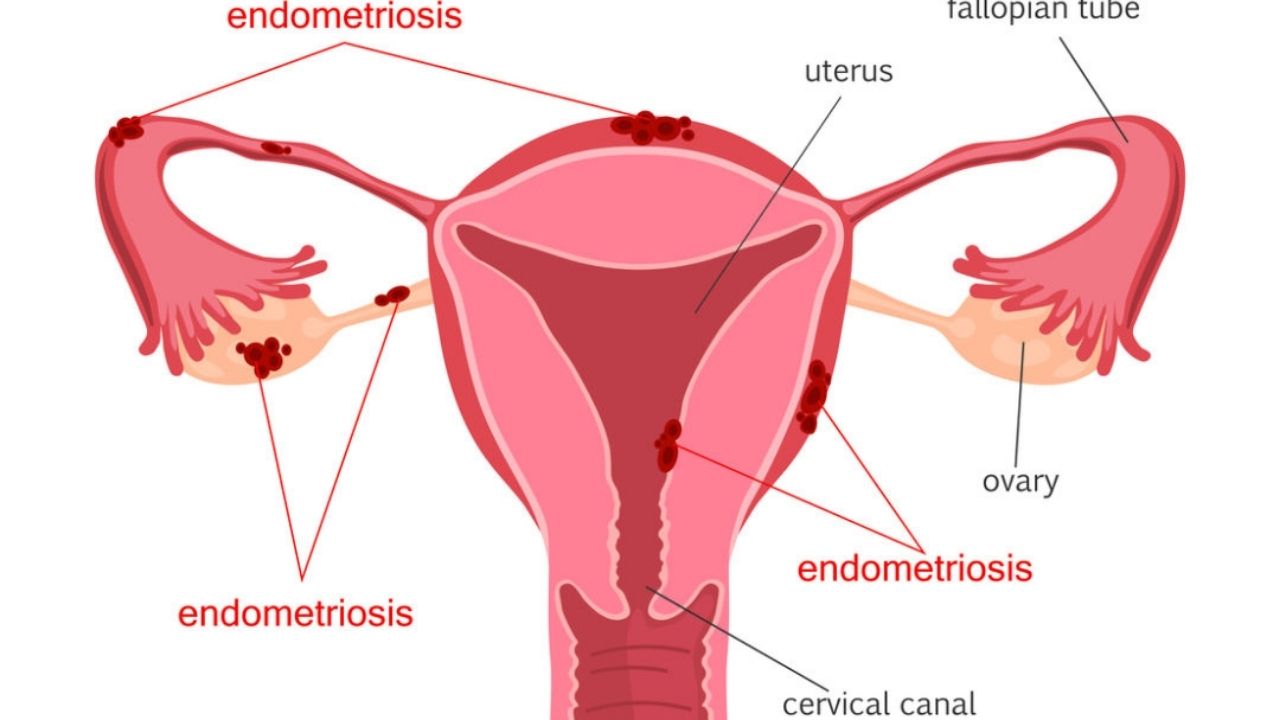
A suspicion of the disease during examination is placed in women of childbearing age (20-45 years), in 10% of cases it can occur in girls after the onset of the first menstruation (menarche) and before the formation of a normal menstrual cycle, as well as in 2-5% in women in menopause … Diagnosis is often difficult due to its asymptomatic course of the disease, which may suggest its greater prevalence. In recent years, with the introduction of new methods of diagnosis and treatment – hysteroscopy and laparoscopy, the rate of detection of endometriosis has increased significantly.
Causes of endometriosis
To date, there is no single version of the causes of endometriosis.
1 theory: “Retrograde menstruation or implantation theory”
Some women have a tendency to have a feature such as retrograde menstruation (when the muscle layer of the uterus contracts in the opposite direction from the cervix). During the period of menstruation (regulation), blood with elements of the endometrium, due to the peristaltic movements of the smooth muscle of the uterus, is brought into the abdominal cavity and fallopian tubes, where the endometrium is implanted into the tissues of various organs. During the normal menstrual cycle, the inner layer of the uterus (endometrium) is separated and excreted from the uterine cavity, while microbleeds occur in other organs affected by endometriotic foci and aseptic inflammation occurs. The likelihood of endometriosis may increase from such reasons as: structural features of the uterine appendages, immune pathological processes, abortions, operations on the uterus, cesarean section,
The role of heredity in the pathology under consideration is especially high and suggests a very high possibility of the occurrence of a disease in a daughter, if her mother had previously suffered such a disease. Knowing about the predisposition to this pathology, a woman, observing preventive measures, can prevent the onset of the disease. So, for example, after surgical interventions on the organs of the reproductive system, a woman needs systematic monitoring of her health to prevent possible complications.
2 theory: “Gene mutations”
3 theory: “Abnormalities in the function of cellular enzymes and the reaction of receptors to hormones”
However, the latter two theories have not received widespread popularization due to the small evidence base. Endometriosis is classified by location.
Endometriosis classification
- Genital. From the name itself, it follows that during the course of the disease in this form, endometriotic foci are located in the tissues of the patient’s reproductive organs.
- Peritoneal (peritoneal) endometriosis – affects the ovaries, pelvic peritoneum, fallopian tubes.
- Extraperitoneal (extraperitoneal) endometriosis occurs in the organs not covered by the peritoneum: in the lower parts of the genitals, the vulva, in the cervix (its vaginal segment), the posterior vaginal septum, etc. In the muscular layer of the uterus, internal endometriosis (adenomyosis) can form, while the uterus spherical in shape and reaches a size up to 5-6 weeks of gestation.
- Extragenital endometriosis. In this form, endometriotic foci are located outside the reproductive system (digestive tract, respiratory system, urinary system, postoperative scars).
- In serious, complicated cases of the disease, endometriosis is mixed.
Depending on the depth and distribution of foci of endometriosis, 4 degrees are distinguished:
- I stage – superficial and single foci;
- II stage – the lesions are deeper and in greater numbers;
- III stage – deep multiple endometriotic foci, as well as endometrioid ovarian cysts, individual adhesions of the peritoneum;
- IV Stage – multiple and deep foci, large endometrioid cysts of both ovaries, extensive adhesions. The endometrium can invade the walls of the vulva and rectum. As a rule, this degree of endometriosis is difficult to treat, characterized by the scale and degree of invasion of the process.
Adenomyosis of the uterus is classified separately – according to the depth of invasion of the pathological process into the muscular layer of the uterus (myometrium):
Stages of endometriosis
- Stage I initial germination of the myometrium;
- Stage II foci of endometriosis germinate to half the depth of the myometrium;
- Stage III completely sprouts the myometrium to the serous membrane of the uterus;
- Stage IV germination of the walls of the uterus with the spread of foci to the serous membrane (peritoneum).
Endometriotic foci are also characterized by other parameters. For example, they can take on various shapes: from rounded to neoplasms that do not have clear outlines, and be different in size – from a few millimeters to several centimeters. As a rule, neoplasms are separated from adjacent structures by adhesions or cicatricial processes and are brown in color.
Depending on the cyclicity of regulation, endometriotic foci mostly appear on the eve of menstruation. The foci have a very different localization and are found not only on the surface of organs, but also show a tendency to deep invasion of the tissue. When the ovaries are involved in the process of endometriosis, the cysts are grouped and filled with bloody contents. Based on the size and depth of endometriotic lesions, as well as the localization of the formations, the degree of endometriosis is determined by the point system.
Symptoms of endometriosis
- Pelvic pain. It occurs in 16-24% of patients. It can have both point and diffuse localization, it arises and increases in correlation with the menstrual cycle, it can be constant. It is often caused by inflammation and adhesions that develop with endometriosis.
- Dysmenorrhea is pain during menstruation. The most common complaint that causes the most suffering and discomfort occurs in 40-60% of women. The maximum manifestations are expressed in the first few days of regulation. Endometriotic foci often bleed into the cavity of the ovarian cyst, increasing their pressure, irritating the peritoneum, causing contraction of the smooth muscles of the uterine blood supply vessels.
- Painful intercourse. Soreness when emptying the bladder or rectum. It is observed in 2-16% of patients. With the localization of endometriotic foci in the pelvic organs in the vulva, uterine-rectal space, in the region of the sacro-uterine ligaments, in the wall of the rectovaginal septum, it can cause discomfort and even pain during intercourse or when emptying the rectum and bladder. These symptoms can also accompany adenomyosis and many other diseases: uterine fibroids, polycystic ovaries, etc.
- Post-hemorrhagic anemia. In 25-40% of patients, due to significant chronic blood loss during menstruation, a state of anemia may occur. Weakness, pallor or yellowness of the skin and mucous membranes, dizziness, fatigue, drowsiness, irritability and mental irritability gradually increase.
- Infertility. Today, scientists and doctors are unable to accurately assess how and why infertility occurs when endometriosis is affected. They associate this with the processes in the uterine appendages with endometriosis, with interruptions in the functioning of the general and local immune status of the organism as a whole, and as a result, failures in ovulatory processes. Not absolute, but rather high with endometriosis, the possibility of not getting pregnant. Endometriosis and its attendant processes can provoke spontaneous abortions, which, in turn, dramatically and significantly reduce the chances not only of pregnancy, but also of its normal course. Therefore, pregnant women with a history of endometriosis should be constantly monitored by a doctor. 15- 56% of patients treated for endometriosis become pregnant within 6-12 months.
Diagnosis of endometriosis
With the introduction of minimally invasive methods of diagnosis and treatment (hysteroscopy and laparoscopy), the detection rate of endometriosis has increased significantly.
Due to the similarity of the course of this disease with other diseases of the genital organs, similar in symptomatology, differential diagnosis is very important at all stages of diagnosis. The doctor carefully collects complaints and anamnesis, information about past diseases, including the reproductive system, surgical operations, the presence of a gynecological and obstetric history of burdened relatives on the female side.
Further examination includes:
- gynecological examination (vaginal, rectovaginal, in the mirrors) is most informative on the eve of menstruation;
- colposcopy and hysterosalpingoscopy to obtain a biopsy from the affected organs and clarify the location and shape of the lesions;
- Ultrasound of the pelvic organs, abdominal cavity to clarify the localization and dynamics in the treatment of endometriosis;
- computed tomography or magnetic resonance imaging to detail the nature, localization of formations and the depth of the lesion;
- laparoscopy, which makes it possible to visualize pathological processes, assess their activity, quantity, and determine the degree of maturity;
- hysterosalpingography (X-ray examination of the fallopian tubes and uterus with the introduction of contrast in their cavity);
- hysteroscopy (endoscopic visualization of the uterine cavity), which makes it possible to diagnose adenomyosis in 83% of cases;
- blood tests for the presence of tumor markers in the endometriotic process increase significantly: CA-125, CEA and CA 19-9, RO-test.
The complex of all methods makes it possible to identify endometriotic foci in up to 96% of cases.
The final diagnosis can be made only if a histological examination of a biopsy specimen from the foci of endometriosis taken during hysteroscopy (laparoscopy) is performed.
Endometriosis treatment
It is very important to take into account the following factors in determining the tactics of endometriosis therapy:
- what age category does the patient belong to,
- the number of pregnancies, including those that ended in childbirth,
- it is important to know how the childbirth proceeded and whether there were any complications in the postpartum period,
- the severity of the pathological process, its location, depth, concomitant pathologies, the desire to have a child are taken into account.
Therapy can be divided into drug treatment, surgical (surgical removal of endometriotic foci with preservation of organ function – laparoscopic or radical extirpation of the uterus and its appendages, as well as combined.
When treating endometriosis, the doctor’s actions are aimed not only at eliminating the manifestations of the disease in question, but also at its consequences (adhesive and cystic formations, neuropsychiatric manifestations, etc.).
Surgical treatment of endometriosis
In moderate and severe stages of endometriosis, it is recommended to resort to organ-preserving surgical treatment with the removal of foci. Treatment is comprehensively aimed at resection of heterotopia in affected organocomplexes, resection of endometrioid cysts in the ovaries, and dissection of adhesions. As a rule, it is used if there is no effect of drug treatment, there are various contraindications, for example, intolerance to drugs or their components, when endometrioid neoplasms larger than 3-4 centimeters are detected, urinary dysfunction, problems with the gastrointestinal tract. Surgical treatment is often combined with drug treatment. The intervention is carried out by laparoscopic or laparotomic approaches.
If the patient’s disease progresses actively after the age of 40 and conservative- surgical measures do not give the desired effect, then they resort to radical surgical removal of endometriosis (extirpation of the uterus with appendages). Such measures are not often used and occur in 12% of patients.
Basic principles of surgical treatment of endometriosis from the standpoint of evidence-based medicine
Regardless of how far and deeply the pathological process has spread, laparoscopy is the preferred surgical approach (“gold standard”) in the treatment of endometriosis. It promotes better visualization of lesions, due to their optical magnification, minimal tissue trauma and faster rehabilitation of patients than after laparotomy. Therapeutic and diagnostic laparoscopy with the removal of endometriotic neoplasms provides a significant reduction in the intensity of pain associated with endometriosis.
Ovarian endometriomas in women with pelvic pain should be surgically removed by laparoscopy.
For women of childbearing age, it is fundamentally important to recover from ovarian endometriosis without the risk of recurrence with the maximum preservation of unaffected oocyte tissue. For this, puncture, drainage of the cyst, alcoholization and destruction of the capsule are performed by exposure to various types of energy. However, all these methods do not completely remove the cyst capsule, which can lead to a relapse of the disease.
In women who are not interested in pregnancy, endometriotic foci can be removed by laparoscopic or combined laparoscopic- vaginal access, if necessary, in combination with simultaneous resection of the affected area of the rectal wall or in a single block with the uterus.
Only the removal of the uterus (extirpation of the uterus) can be considered a radical method of treating adenomyosis. This operation is usually performed laparoscopically. When performing surgery to remove the uterus, it is very important to remove all visible endometriotic lesions, while bilateral removal of the ovaries can contribute to more effective disappearance of pain and reduce the likelihood of recurrence of the disease.
The question of removing the ovaries should be discussed with each patient individually.
Conservative treatment is used if endometriosis has a latent course, the patient’s age is up to 45 years, during premenopause, and there is a need to preserve reproductive function.
Hormone therapy in the treatment of endometriosis
- Combination therapy with estrogens and progestogens. According to the recommendations, combined oral contraceptives – COCs (hormonal contraceptive pills) are most preferable for the elimination of pelvic pain in women who are not planning a pregnancy and have no contraindications to their use. The main advantages of COCs are their relatively low cost, low risk of side effects and the acceptability of the duration of therapy. The use of COCs significantly reduces the intensity of pain associated with endometriosis. Continuous use of COCs has priority in the treatment of endometriosis in comparison with the cyclic regimen. The drugs help to reduce the intensity of pain after 6 months. by 58%, and after 2 years – by 75% in patients with severe dysmenorrhea.
- Progestogens (byzanne, norkolut, MPA, dyufaston, levonorgestrel). This group of drugs can be recommended for therapy at various stages of the disease. Patients are prescribed reception in a continuous course from 6 to 8 months. How side effects can appear: in the intermenstrual period, spotting, psychological depression, increased sensitivity of the mammary glands.
- Antigonadotropic drugs (danazol, danogen, danol, etc.). Suppress the production of gonadotropins in the hypothalamic-pituitary system. They are taken continuously, as a rule, for at least six months. A contraindication is hyperandrogenism (excess of androgenic hormones). How side effects can appear: sweating, a feeling of heat, weight fluctuations, a decrease in voice tone, increased greasiness of the skin, intense hair growth.
- Agonists of gonadotropic releasing hormones (triptorelin, goserelin, etc.). A positive point when using drugs in this group is the possibility of a single dose per month and the absence of severe side effects. Agonists of releasing hormones cause inhibition of ovulation and a decrease in estrogen in the body, which leads to restraining the spread of endometriotic neoplasms.
- In addition to hormonal drugs, immunostimulating drugs are used in the treatment of this pathology , as well as symptomatic therapy: antispasmodics, pain relievers. With severe pain syndrome, non-steroidal anti-inflammatory drugs (diclofenac, indomethacin, voltaren), antidepressants, psychotherapy are used.
Full convalescence with endometriosis occurs only with its early detection and high-quality subsequent therapy.
Estimated indicators of recovery from endometriosis are: good health, no complaints of pelvic pain, no relapse within 5 years after therapy, recovery or maintenance of fertility.
With the current level of development of surgical gynecology with the extensive use of organ-preserving methods of treatment, all of the above can be achieved in 60% of women aged 20 to 36 years. If the patient was assisted in the form of a radical operation, then the disease does not recur.
Complications of endometriosis
- Endometrioid ovarian cysts (“chocolate” cysts) filled with old menstrual blood.
- Hemorrhages and cicatricial changes.
These two complications are highly likely to lead to a state of infertility. Extensive and widespread endometriotic foci put pressure on the nerve trunks and endings, which leads to a variety of neurological disorders. Malignancy of degenerated foci of endometriosis is rare. According to scientists, in women with endometriosis, the risk of developing oncological transformations is 50% higher than the average.
Prevention of endometriosis
The earlier, when the first symptoms of endometriosis appear, a woman comes for a consultation with a gynecologist, the higher the chance of completely eliminating the need for surgical treatment. Attempts to self-therapy or postponement of seeking help are completely unjustified: with the next menstrual cycle, new endometriotic foci appear, cysts appear, cicatricial and adhesions intensify, and the condition of the fallopian tubes is aggravated.
For the prevention of endometriosis, you must:
- examination of adolescent girls and women with complaints of pain during menstruation;
- supervision of patients after abortions and other other manipulations on the uterus to eliminate possible consequences;
- timely and complete elimination of acute and chronic pathologies of the genitals;
- taking oral hormonal contraceptives.
The risk of endometriosis is higher in women who smoke after the age of 30-35 years with a short menstrual cycle, suffering from metabolic disorders, obesity, overweight; having intrauterine contraceptives; with an increased level of estrogen; suffering from immunosuppression; having a hereditary predisposition and having undergone surgery on the uterus.