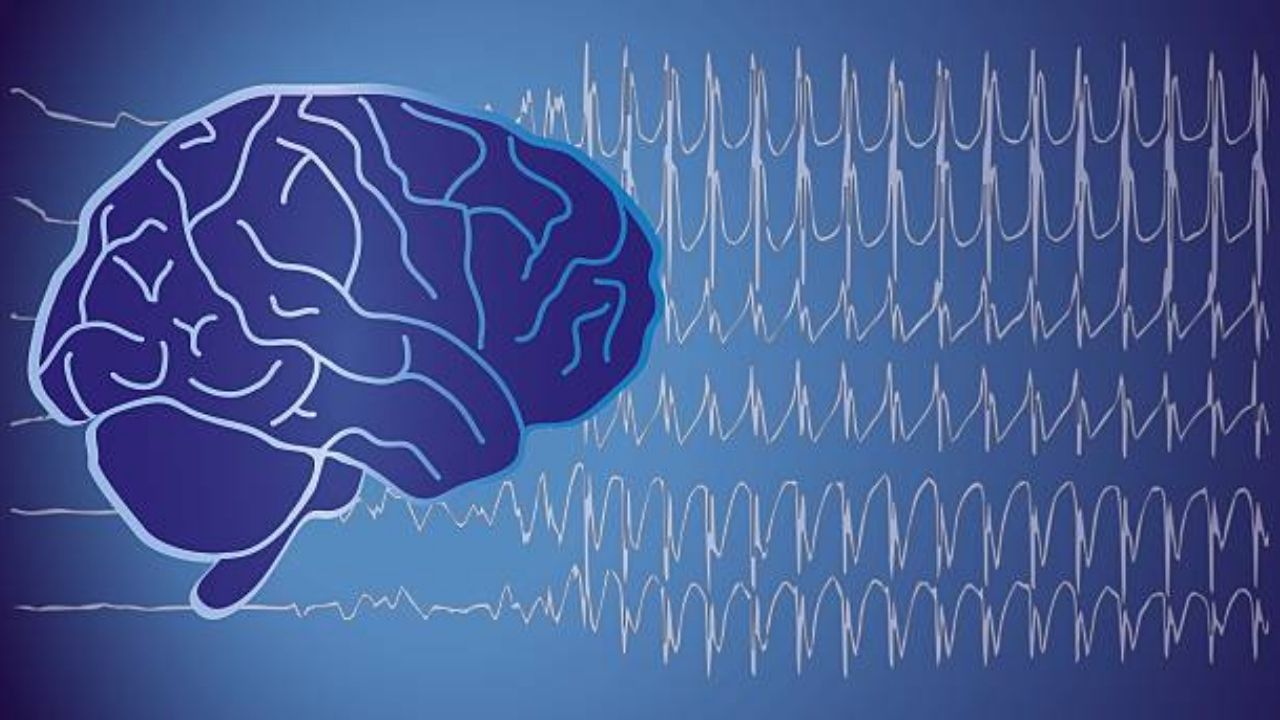
Epilepsy is a malfunction of the brain. It is triggered by nerve cells that suddenly simultaneously fire impulses and discharge themselves electrically.
ICD codes for epilepsy: G40 | G41
Quick overview
• Description: Epilepsy is characterized by epileptic seizures. These are short-term functional disorders of the brain in which nerve cells are electrically discharged in an extreme form.
• Types: There are different types of seizures and forms of epilepsy, for example generalized seizures (such as absences or “grand mal”), focal seizures, rolandic epilepsy, Lennox-Gastaut syndrome, West syndrome, etc.
• Causes: partly unknown, partly due to another disease (brain damage or inflammation of the epidermis, concussion, stroke, diabetes, etc.). Very often, the combination of genetic predisposition and another disease leads to the development of epilepsy, experts believe.
• Treatment: usually with medication (antiepileptics). If these don’t work well enough, sometimes surgery or electrical stimulation of the nervous system (such as vagus nerve stimulation) are treatments.
What is epilepsy?
Epilepsy (“falling sickness”) is one of the most common temporary functional disorders of the brain. It is characterized by epileptic seizures: nerve cells (neurons) in the brain suddenly fire synchronously and uncontrolled impulses for a short time.
Such an attack can vary in severity. The effects are correspondingly variable. For example, some patients only feel a slight twitching or tingling of individual muscles. Others are briefly “out of the way” (absent). In the worst case, there is an uncontrolled seizure of the whole body and a brief loss of consciousness.
Epilepsy: definition
According to the International League Against Epilepsy (ILAE), epilepsy is diagnosed when:
• At least two epileptic seizures occur more than 24 hours apart. Most often, these seizures come “out of nowhere” (unprovoked seizures). On the other hand, in rarer forms of epilepsy, triggers for the seizures can be identified, such as light stimuli, noise or warm water (reflex seizures).
• While only one unprovoked or reflex seizure occurs, there is at least a 60 percent chance of having more seizures in the next ten years. It is therefore just as great as the general risk of recurrence after two unprovoked seizures.
• There is a so-called epilepsy syndrome, for example the Lennox-Gastaut syndrome (LGS). Epilepsy syndromes are diagnosed on the basis of certain findings that include, for example, the type of seizure, electrical brain activity (EEG), the result of imaging tests and the age of onset.
So-called occasional seizures must be distinguished from this “real” epilepsy. These are individual epileptic seizures that can occur in the course of various diseases. As soon as the acute illness subsides, these occasional cramps also stop. An example of this is febrile seizures: these epileptic seizures occur in connection with fever, especially in young children. However, there is no evidence of a brain infection or any other specific cause.
In addition, occasional cramps can occur, for example, with severe circulatory disorders, poisoning (with medication, heavy metals), inflammation (such as meningitis), concussion or metabolic disorders.
Types of epilepsy
There are many different types and characteristics of epilepsy. The classifications in the specialist literature vary, however. A commonly used (rough) classification is as follows:
• Generalized epilepsies and epilepsy syndromes: Here the seizures cover the entire brain. Depending on the type of seizure, generalized seizures are further divided into, for example, tonic seizures (limbs cramp and stiffen), clonic seizures (slow jerking of large muscle groups), or tonic-clonic (“grand mal”) seizures.
• Focal epilepsies and epilepsy syndromes: Here the seizures are limited to a limited area of the brain. The symptoms of the seizure depend on its function. For example, twitching of the arm (motor seizure) or changes in vision (visual seizure) are possible. In addition, epilepsy can begin focally, but then spread to the entire brain. This is how it develops into a generalized seizure.
In addition to these two large groups of epilepsies, there are also seizures of unclear onset and unclassifiable epileptic seizures.
Epileptical attack
During an epileptic seizure, either the whole brain (generalized seizure) or a specific area of the brain (focal seizure) suddenly becomes overactive. The whole thing often only takes a few seconds, sometimes a little longer. As a rule, however, an epileptic seizure is over after two minutes at the latest.
An epileptic seizure is very often followed by an after-phase: although the brain cells are no longer pathologically electrically discharged, abnormalities can still appear for up to several hours. These include, for example, a disturbance in attention, speech disorders, memory disorders or aggressive states.
However, sometimes people recover completely after an epileptic seizure after just a few minutes.
First aid
An epileptic seizure can be disturbing to outsiders. In most cases, however, it is not dangerous and ends on its own within a few minutes. If you witness an epileptic seizure, you should follow the following rules to help the patient:
- Keep Calm!
- Don’t leave the patient alone, calm him down!
- Protect the patient from injury!
- Do not hold the patient!
Epilepsy in children
Epilepsy very often occurs in childhood or adolescence. It is one of the most common diseases of the central nervous system in this age group. In Germany and other industrialized countries, around 50 out of 100,000 children develop epilepsy every year.
Taking medication regularly can usually prevent further epileptic seizures in young patients. A healthy lifestyle is also important: If the epileptic seizures are “triggered” by certain triggers (such as lack of sleep, flickering lights, certain noises, etc.), these should be avoided as far as possible.
Overall, epilepsy in children is easily treatable in many cases. And the concern of many parents that epilepsy could impair their child’s development is mostly unfounded.
Symptoms of epilepsy
The exact symptoms of epilepsy depend on the form of the disease and the severity of the epileptic seizures. For example, the mildest variant of a generalized seizure consists only in a short-term mental “absence” (absence): the patient has “gone away” briefly.
At the other end of the scale is the “big seizure” (grand mal): First, the whole body cramps and stiffens (tonic phase). Then he begins to twitch uncontrollably (clonic phase). During such a tonic-clonic seizure, patients are unconscious.
Another severe type of epilepsy is the so-called “status epilepticus” : This is an epileptic seizure that lasts longer than five minutes. Sometimes there is a series of seizures in rapid succession without the patient regaining full consciousness in between. Such situations are emergencies that must be treated as quickly as possible by the emergency doctor!
Cause and risk factors of epilepsy
The development of epilepsy is diverse and complex. The exact development of the disease often remains in the dark. In some cases, despite modern examination methods, no specific cause can be identified for epileptic seizures, although there are clear indications of a cause in the brain. Then one speaks of unexplained (cryptogenic) epilepsy.
Sometimes it is not even possible to explain why a patient has epileptic seizures. There is no evidence of the cause, such as pathological changes in the brain or metabolic disorders. This is what doctors call idiopathic epilepsy.
Recently, however, this term has been (at least partially) replaced by ” genetic epilepsy “: Many sufferers probably or demonstrably have genetic changes, for example at binding sites (receptors) for neurotransmitters. According to experts, such genetic changes can contribute to the development of epilepsy. It is therefore usually not hereditary. Parents usually only pass on the susceptibility to seizures to their children. The disease only occurs when external factors come into play (such as sleep deprivation or hormonal changes).
Finally, with regard to the causes, there is another group of epilepsies: In many patients, structural changes in the brain or underlying diseases can be identified as the cause of the epileptic seizures. Doctors refer to this as symptomatic epilepsy or – according to more recent proposals – as structural/metabolic epilepsy. This includes, for example, epileptic seizures that are based on congenital malformations of the brain or brain damage acquired at birth. Also craniocerebral trauma, brain tumors, stroke, inflammation of the brain (encephalitis) or the meninges (Meningitis) and metabolic disorders (diabetes, thyroid diseases, etc.) are among the possible causes of epilepsy.
Sometimes epilepsy is both genetic and structural/metabolic. For example, in some people with a genetic susceptibility to epileptic seizures, epilepsy is only triggered by a stroke, meningitis, poisoning or another specific disease.
Diagnosis of epilepsy
Anyone who experiences an epileptic seizure for the first time should be examined by a doctor. This can determine whether it is actually epilepsy or whether the seizure has other reasons. The first point of contact is usually the family doctor. If necessary, he will refer the patient to a specialist in nerve diseases (neurologist).
Initial consultation
The first step on the way to diagnosing “epilepsy” is taking the medical history (anamnesis): To do this, the doctor talks to the patient (if old enough) and accompanying persons (such as parents, partners) in detail. He allows the epileptic seizure to be described in detail. Here it is an advantage if people are present during the conversation who have had the seizure are present during the conversation. The person concerned often cannot remember it well. Based on the descriptions, the doctor can assess the seizure pattern (seizure anamnesis).
Sometimes there are photos or video recordings of the epileptic seizure. They can be very helpful to the doctor, especially when the focus is on the patient’s face. The eyes are important seizure symptoms and help distinguish an epileptic seizure from other seizures.
During the conversation, the doctor also asks about possible triggers of the seizure (such as flickering lights), possible underlying diseases and known cases of epilepsy in the family.
Investigations
The interview is followed by a physical examination. The state of the nervous system is also checked using various tests and examinations (neurological examination). This includes one measuring the brain waves (electroencephalography, EEG): Sometimes epilepsy can be recognized by typical curve changes in the EEG. However, the EEG in epilepsy can also be unremarkable.
Magnetic resonance imaging (MRI or magnetic resonance imaging) is very important in the clarification of an epileptic seizure. Detailed cross-sectional images of the brain are created. The doctor can then identify any damage or malformations of the brain as a possible cause of the seizure.
In addition to the MRI, a computed tomography of the skull is sometimes made. Computer tomography can be used especially in the acute phase (shortly after the attack). can help to discover, for example, cerebral hemorrhage as the cause of the attack.
Laboratory tests can provide clarity if brain inflammation (encephalitis) or another underlying disease is suspected as the cause of the epileptic seizure. A blood test can provide indications of inflammation or metabolic changes. If the doctor suspects drug use as the cause of the seizure, appropriate blood tests are done.
The doctor can also use a fine hollow needle to take a sample of the cerebrospinal fluid from the spinal canal (liquor or lumbar puncture). The analysis in the laboratory helps, for example, brain or meningitis (encephalitis, meningitis) or a brain tumor detect or rule out.
In individual cases, further examinations may be necessary, for example to rule out other types of seizures or to clarify the suspicion of certain underlying diseases.
Treatment of epilepsy
The long-term treatment of epilepsy patients is usually carried out by a registered neurologist or child and adolescent neurologist. Sometimes it can also make sense to go to an outpatient facility or clinic that specializes in epilepsy treatment (specialist practice for epilepsy, epilepsy outpatient clinic, epilepsy center). This applies, for example, if the diagnosis is unclear, epileptic seizures occur despite treatment, or special problems are related to epilepsy.
Epilepsy: therapy is not always necessary
Has anyone (so far) only had one epileptic seizure, treatment can often be delayed. In some cases, it is sufficient if patients avoid known triggers (such as loud music, flickering lights, computer games) and adopt a healthy lifestyle. These include, among other things, a regular lifestyle, regular and sufficient sleep and not drinking alcohol.
In addition, patients should be particularly cautious in situations where a sudden seizure could have dire consequences. This applies, for example, to extreme sports, scaffolding work and when handling heavy machinery. If possible, epileptics should avoid such situations.
In structural/metabolic epilepsy, the doctor first treats the underlying disease (meningitis, diabetes, liver disease, etc.). Here, too, patients should avoid all factors that can trigger an epileptic seizure.
Sometimes, however, treatment with epilepsy medication is advisable even after a single seizure. This may be the case, for example, if the patient has a high risk of further seizures. Drug therapy should also begin immediately in the case of very specific forms of epilepsy (such as Lennox-Gastaut syndrome, temporal lobe epilepsy, etc.).
In general, doctors recommend epilepsy treatment after the second seizure at the latest.
In general, however, it always depends on the situation of the individual patient when and how epilepsy is treated. For example, some patients only have an epileptic seizure every few years. Others have more frequent seizures, which they perceive as less stressful (e.g. only short “pauses” = absences). Then the doctor will carefully weigh up the benefits and risks of epilepsy treatment. In doing so, he also takes into account how willing the patient is to follow medical recommendations (adherence to therapy). There is little point in prescribing medication if the patient does not (regularly) take it after all.
Medication
Drug treatment helps most people with epilepsy to lead a seizure-free life. So-called antiepileptic drugs are used. They inhibit the excessive activity of nerve cells in the brain. This can reduce the risk of a seizure. That is why they are also called anticonvulsants (= anticonvulsants). However, the drugs cannot do anything against the cause of epilepsy. This means: antiepileptic drugs only have a symptomatic effect, but cannot cure epilepsy.
Various active ingredients are used as antiepileptics, for example levetiracetam or valproic acid. The doctor will select an active ingredient for each patient that is likely to work best in the specific case. The type of seizures or the form of the epilepsy plays an important role. In addition, the doctor takes possible side effects into account when choosing the antiepileptic drug and its dosage. The goal is for the treatment to prevent (or at least reduce the number of) future seizures. At the same time, the drug should cause no or only tolerable side effects.
As a rule, the doctor prescribes only one antiepileptic drug (monotherapy) for epilepsy. If this drug does not have the desired effect or causes severe side effects, the doctor may try switching the patient to another drug. Sometimes several preparations have to be tried out before the individually “best” antiepileptic is found.
In some patients, epilepsy cannot be adequately controlled with monotherapy. Then the doctor can prescribe two (or more) antiepileptic drugs. Such combination therapy is carefully planned and monitored. In general, the more different medications someone takes, the more likely it is that undesirable interactions can occur. The risk of side effects may also increase.
The epilepsy medications are often taken as tablets, capsules or juice. Some can also be given as an injection, IV, or suppository.
Antiepileptic drugs can only help if they are used regularly. It is therefore very important to follow the doctor’s instructions exactly!
How long do you have to use antiepileptic drugs?
Antiepileptic drugs are usually taken for several years. If, thanks to treatment, no more epileptic seizures have occurred for a long time, patients can sometimes try to stop taking the drug after talking to their doctor. But this must not happen suddenly. Instead, the dosage should be reduced gradually as recommended by the doctor.
In some patients, the epileptic seizures then return (sometimes only after months or years). Then the epilepsy medication must be taken again. Other patients remain permanently seizure-free even after stopping antiseizure drugs. This can happen, for example, if the cause of the seizures (such as meningitis = meningitis) has now healed.
This cannot be predicted in individual cases. The attending doctor can only estimate the risk of seizures without medication based on the individual situation of the patient. In some cases, epileptics have to be prepared from the start that they will probably need the medication for life – for example if permanent brain damage is the cause of the epilepsy.
Never stop taking your epilepsy medication on your own – it can be life-threatening!
Epilepsy surgery
In some patients, epilepsy cannot be adequately treated with medication. If the seizures always start in a limited region of the brain (focal seizures), this part of the brain can be surgically removed (resection, resective surgery). This can in many cases prevent future epileptic seizures.
However, resective surgery is only possible under certain conditions. It must be relatively safe to cut out the relevant brain region. In addition, it must not entail any unacceptable disadvantages for the patient, such as a serious impairment of certain brain functions.
Resective brain surgery is performed primarily in patients in whom the epileptic seizures originate in the temporal lobe of the brain.
More rarely, other surgical procedures are performed in severe epilepsy. This can be the case, for example, with patients who frequently experience severe seizure attacks – i.e. epileptic seizures in which they fall in a flash and may seriously injure themselves. A so-called bar severing (callosotomy) can be considered here: The surgeon cuts through the so-called bar (corpus callosum) in the brain completely or partially. This is the link between the right and left hemispheres of the brain. This intervention can significantly reduce the number of falls. However, there is a risk of cognitive impairment as a side effect. Therefore, the benefits and risks of callosotomy must be carefully weighed against each other.
Stimulation procedure
In addition to an operation, so-called stimulation procedures can also be considered if medication for epilepsy is not effective enough. Certain structures in the brain or those that lead there (vagus nerve) are stimulated with a low current. This can help against epileptic seizures.
There are a number of different methods that can be used to treat epilepsy. The most common is vagus nerve stimulation (VNS) : A small, battery-operated device is implanted under the patient’s skin below the left collarbone. It is a type of pacemaker that connects to the left vagus nerve in the neck via a wire that also runs under the skin. At intervals (for example, every five minutes for 30 seconds), it delivers gentle shocks of electricity to the nerve. This can significantly reduce the frequency of epileptic seizures. In some patients, however, it takes a few months for this effect to set in.
During the current pulses, some patients experience hoarseness, coughing or abnormal sensations (“buzzing” in the body).
Vagus nerve stimulation can also have a positive effect on co-existing depression.
Another stimulation method is deep brain stimulation : Small electrodes are implanted in the patient at certain points in the brain. They stimulate the nerve tissue with electrical impulses. As a result, the number of seizures decreases in many patients. Possible side effects include depression and memory problems. Deep brain stimulation should only be performed in specialized centers.
Treatment for status epilepticus
If someone suffers status epilepticus, bystanders should immediately call the emergency doctor – there is a risk of death! The patient is first given a sedative (benzodiazepine). It can also be administered by laypersons if the epileptic is carrying the emergency medication with them: it is either placed in the cheek (buccal tablet) or inserted as a cream into the patient’s anus via a small tube. The emergency doctor who arrives can also administer the sedative as an injection into a vein. He then rushes the patient to a hospital. The treatment will continue there.
If the status epilepticus still cannot be ended after 30 to 60 minutes, many patients are given anesthesia and artificial respiration.
Course and prognosis of epilepsy
The course and prognosis of epilepsy depend on the type of seizure and the type of epilepsy. There are also differences from patient to patient. In general, about half of the patients have a single epileptic seizure. The other half will have another seizure sooner or later. After that, the risk of seizures continues to rise: about seven out of ten patients who have already had two attacks have another epileptic seizure within a year.
People whose epilepsy is caused by an underlying disease such as a brain disease are particularly at risk: The risk of further seizures is about twice as high in them as in patients whose epilepsy is based on a genetic predisposition or has no known cause.
Avoid seizures
With the right and consistent treatment, further epileptic seizures can be avoided in most cases. But patients can do more to prevent seizures. Many of those affected benefit from sufficient sleep with regular sleep times (sleep hygiene).
Sometimes epileptic seizures are provoked by certain triggers. Then patients should avoid them as much as possible. But that only works if you know the triggers. A seizure calendar can help here: the patient notes the day, time and type of each individual seizure along with the current medication intake. Accompanying circumstances and possible triggers are also recorded, for example computer work, loud music, alcohol consumption, sleep deprivation, emotional stress or the sight of certain optical patterns (such as a checkerboard pattern). This helps doctor and patient to identify the trigger factors.
Living with epilepsy
If epilepsy is well controlled with treatment, you as a patient can lead a largely normal life. However, you should take a few precautions to avoid dangerous situations:
- Do not use electric knives or slicers.
- Avoid bathing and take a shower instead. Also, never go swimming unaccompanied. Death by drowning is about 20 times more common in epileptics than in the general population!
- Always ride your bike with a helmet and prefer routes with little traffic.
- Choose a low bed (risk of falling).
- Secure sharp edges in the home.
- Keep a safe distance from roads and bodies of water.
- Don’t lock yourself in. Use a “busy” sign in the restroom instead.
- Don’t smoke in bed!
Whether you, as an epilepsy patient, are allowed to get or keep your driving license depends on whether you are fit to drive. Ask your neurologist for advice on this. He or she can best assess how high your risk of seizures is.
Epilepsy patients who get behind the wheel even though they are unfit to drive endanger themselves and others! They also risk their insurance coverage.
Most jobs and sports are generally also possible for epileptics – especially if, thanks to therapy, epileptic seizures no longer occur. In individual cases, the doctor treating you is best able to assess whether the patient should avoid a certain activity or sport. He may also be able to recommend special precautions.
Epilepsy: contraception & desire to have children
Some epilepsy medications reduce the effectiveness of birth control pills. Conversely, the pill can also impair the effectiveness of some antiepileptic drugs. Girls and women with epilepsy should discuss such interactions with their doctor. He may recommend another contraceptive.
If women with epilepsy want to have children, they should definitely discuss this with their neurologist – preferably before they become pregnant. The drug treatment for epilepsy may have to be adjusted during pregnancy. In higher doses, antiepileptic drugs can disrupt the development of the child or cause birth defects (up to the 12th week of pregnancy). This risk is also higher with combination therapy (several antiepileptic drugs) than with monotherapy (treatment with a single antiepileptic drug). The doctor will take this into account when planning the therapy.
A special feature also applies to folic acid preparations, which are recommended to all women during pregnancy: some antiepileptic drugs lower the folic acid level in the body. Therefore, epileptics should possibly take folic acid in higher doses.
If an epileptic seizure occurs during pregnancy, there is usually no particular reason for concern: the seizure usually does not harm the unborn child – unless it is a long-lasting, generalized seizure, or the expectant mother is seriously injured. But that only happens very rarely. In general, seizures are not very common during pregnancy : around two-thirds of all epileptics remain seizure-free for the entire nine months. In addition, most women with epilepsy give birth to healthy children.
Epilepsy awareness month

Epilepsy is a neurological disorder that affects 3 million Americans and nearly 65 million people worldwide. Those spontaneous seizures that affect people of all ages are the hallmark of epilepsy. In the United States, November is National Epilepsy Awareness Month.