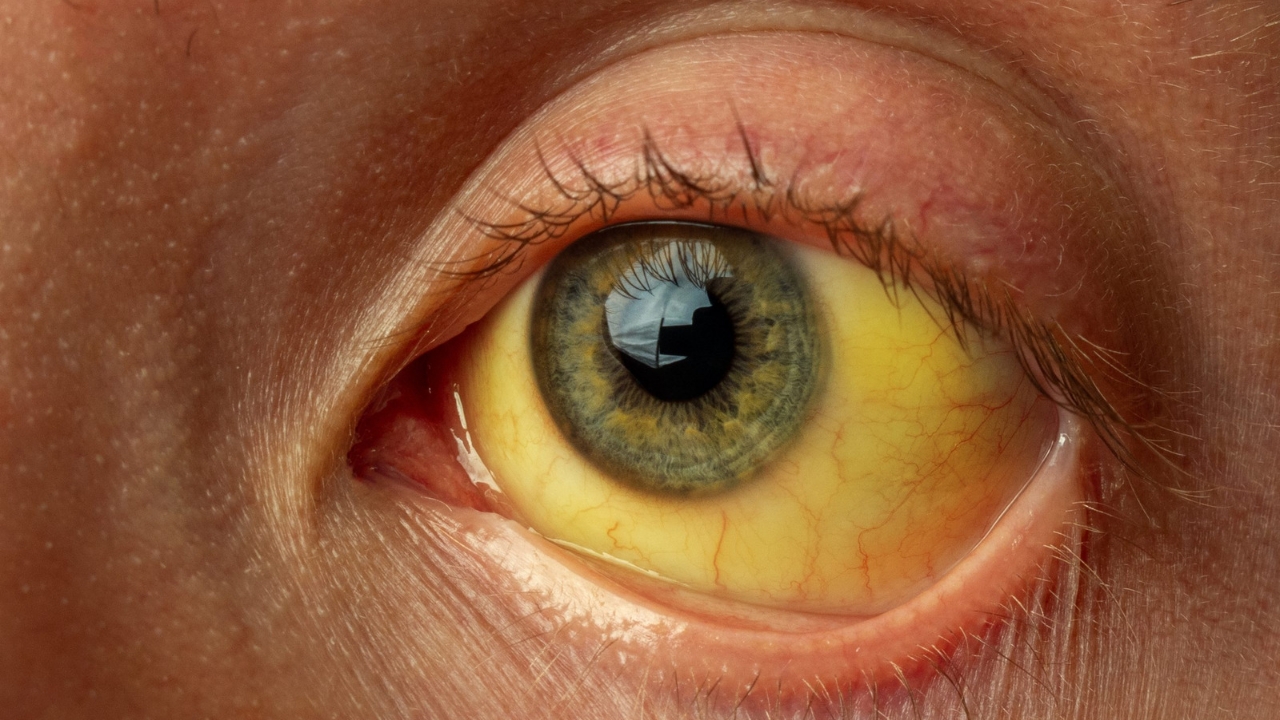
In jaundice, the skin, mucous membranes and the dermis of the eyes turn yellow. The bilirubin is responsible for this.
The yellowish-brown pigment is produced when old red blood cells are broken down. Usually it is excreted in the stool and urine.
However, various diseases can interfere with this process, causing bilirubin to build up in tissue and discolor it.
Read everything you need to know about jaundice, its causes and treatment options here.
Overview
- Description: Yellowing of the skin , mucous membrane and dermis of the eyes due to deposited bilirubin. The yellowish-brown pigment is a by-product of the breakdown of old red blood cells.
- Causes: e.g. liver inflammation (hepatitis), liver cirrhosis , liver cancer and liver metastases , gallstones, biliary tumor, sickle cell anemia , artificial heart valves, right heart failure, poisoning, certain drugs.
- When to the doctor Always – especially if there are other warning signals in addition to yellowing of the skin, mucous membrane or eyes, such as light-colored stools or fatty stools, dark urine, tiredness, exhaustion, loss of performance, loss of appetite, unwanted weight loss, ascites, fever, confusion, disorientation, severe Bad breath.
- Diagnosis: Interview to collect the medical history (anamnesis), physical examination, blood test, imaging tests such as ultrasound .
- Prevention: moderate alcohol consumption, low-fat diet, vaccination against hepatitis, follow health recommendations when traveling to countries at risk of hepatitis.
Jaundice: description
Jaundice is not a disease, but a symptom. It denotes yellowing of the skin, mucous membranes and eyes. Inflammation of the liver (hepatitis) is often mistakenly equated with jaundice.
The breakdown of red blood cells (erythrocytes) plays a role in the development of jaundice:
The red blood cells have a lifespan of around 120 days. Then they are broken down in the liver and spleen . This creates what is known as bilirubin as a by-product. The yellowish-brown dye is insoluble in water.
So that it can be transported with the blood, it is attached to the large protein molecule bound albumin – doctors then speak of indirect bilirubin.
The bilirubin is released in the liver and made water-soluble by binding to glucuronic acid. In this form it is called direct bilirubin.
Then it goes on towards the gallbladder , where the direct bilirubin mixes with the bile. In the course of digestion, bile with the bilirubin contained in it is released via the bile duct to the duodenum and further into the intestine, if necessary.
A large part of the previous bilirubin is excreted in the stool in an altered form, which explains its brown color. Another part leaves the body in the urine, which appears yellow as a result.
Bilirubin build-up in tissues
The level of bilirubin in the blood is usually low. However, certain factors can increase bilirubin levels. If the values rise to more than 2 mg / dl (milligrams per deciliter), the dye is deposited in the tissue.
This is first and foremost visible in the eyes: the normally white leather skin turns yellow. If the bilirubin concentration in the blood continues to rise, the skin and mucous membranes also turn yellow.
In addition to yellowing, itching is characteristic of jaundice. In severe hyperbilirubinemia, even the organs can be discolored yellow.
Causes of jaundice
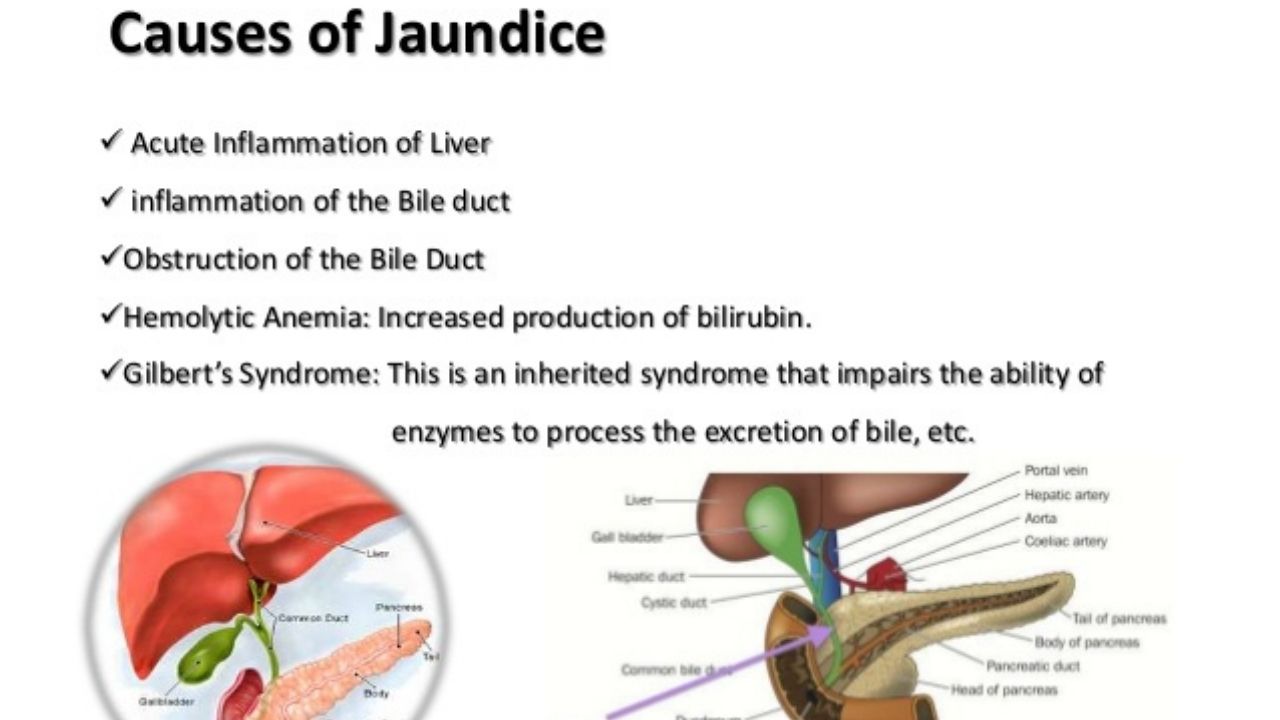
The liver plays an important role in the development of jaundice, as the bilirubin is chemically processed there and passed on to the gallbladder for further processing. However, liver disease is not always the cause of jaundice.
The causes are therefore divided into three aspects:
1. Hemolytic jaundice (prehepatic jaundice)
If the liver does not manage to break down indirect bilirubin quickly, it is deposited in the tissue – the skin and eyes are typically yellowed.
Since the cause is not in the liver itself, but in upstream processes, doctors also refer to this jaundice as “pre-hepatic”.
Blood diseases in which the red blood cells do not live as long as normally and are therefore increasingly broken down are responsible for this.
Sickle cell anemia is an example of such a disease. But artificial heart valves, viral infections, poisons and certain drugs can also reduce the lifespan of the red blood cells.
2. Hepatic jaundice
The liver plays a central role in processing bilirubin. She chemically converts it and sends it to the gallbladder. Various diseases can severely disrupt these processes.
If the liver is no longer able to continue processing, the bilirubin builds up in the blood and is finally deposited in the tissue. The causes of this liver-related jaundice are many:
- Viral hepatitis: Hepatitis viruses (hepatitis A , B, C, D or E) often cause acute liver inflammation. Symptoms include tiredness, weight loss, fatigue, vomiting, nausea , abdominal pain, and jaundice . The discoloration of stool and urine is also typical: the stool is light-colored, the urine dark in color. If acute hepatitis turns into chronic hepatitis, cirrhosis and liver cancer can result. To this day, hepatitis B is one of the most common infectious diseases of mankind. Vaccinations against hepatitis A and B can protect against infection.
- Liver cirrhosis: Chronic liver disease can alter the surface of the liver. The organ is then remodeled with extensive scarring. The liver can do its job less and less. The main causes of cirrhosis of the liver are alcohol addiction and viral hepatitis. Symptoms appear very late, but if left untreated, they lead to death. The only therapy is a liver transplant.
- Liver cancer (hepatocellular carcinoma): Liver tumors are often recognized late. They can lead to upper abdominal pain, jaundice, and ascites.
- Liver metastases: The liver is the central organ of the body’s metabolism. If there is a cancerous tumor somewhere in the body (e.g. in the intestine), daughter settlements often arise in the liver.
- Poisoning: Consumption of poisonous mushrooms or toxic chemical substances can seriously damage the liver – up to and including liver failure.
- Medicines: Many medicines are processed in the liver and can cause temporary jaundice.
- Pregnancy: Yellow eyes and yellow skin during pregnancy can indicate pregnancy intoxication (gestosis). But it can also be a fatty liver.
- Right heart failure: If the heart is on the right side, the blood can back up into the liver and damage the cells there. Those affected develop mild jaundice with yellow eyes and water retention in the legs and stomach.
- Pfeiffer’s glandular fever: This infection caused by the Epstein-Barr virus is also called infectious mononucleosis or kissing disease. It is usually associated with swollen lymph nodes, fatigue, fever, sore throat and tonsillitis and an enlarged spleen. Sometimes inflammation of the liver and jaundice also develop.
- Yellow fever: The mosquito-borne yellow fever virus is widespread in tropical areas. In severe cases, liver failure and jaundice can occur, among other things. The disease is then often fatal.
- Congenital increases in bilirubin levels: Some people have hyperbilirubinemia from birth. This is the case, for example, with the harmless Meulengracht’s disease. Those affected produce too little of the liver enzyme responsible for bilirubin processing. The result is jaundice with yellow eyes or yellowish to bronze-colored skin. Otherwise, those affected have no complaints. The disease does not have to be treated by a doctor.
3. Cholestatic jaundice (posthepatic jaundice)
Here a blockage of the main bile duct (ductus choledochus) is responsible for the jaundice: The bile with the bilirubin accumulates in the gall bladder and cannot drain into the duodenum.
Since the disorder only occurs here after the bilirubin has passed through the liver, it is also known as “post-hepatic jaundice”.
The following causes can impede the outflow of bile:
- Gallstones in the gallbladder or bile duct: women over 40 are particularly affected. In addition to jaundice, colic-like abdominal pain, nausea and vomiting are typical symptoms of gallstones. Gallstones can develop into inflammation of the gallbladder (cholecystitis) or inflammation of the pancreas (pancreatitis) in the long term.
- Tumors the gallbladder, duodenum, or pancreas can also block the bile duct. Jaundice usually occurs in those affected before other symptoms arise.
Signs and symptoms of jaundice
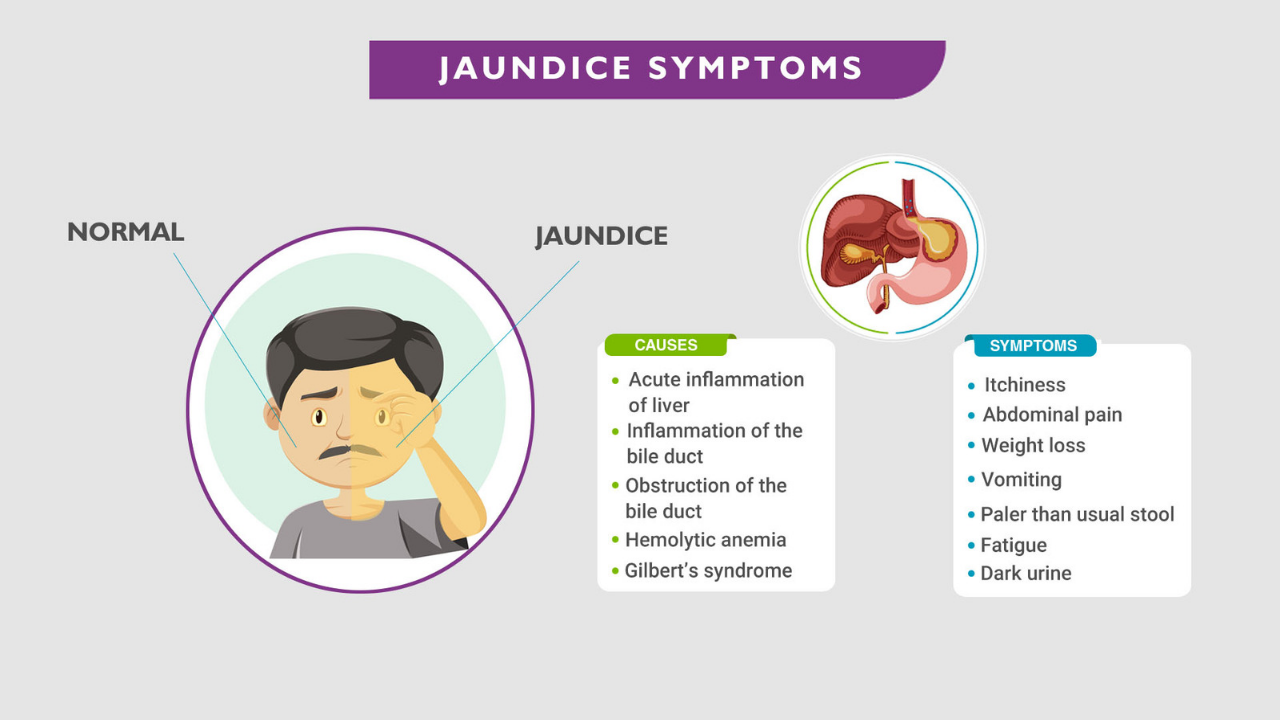
Jaundice: when do you need to see a doctor?
Yellow skin, mucous membranes or eyes are alarming and should always be examined by a doctor. This is especially true if there are other typical jaundice symptoms:
- Discoloration of stool and urine: The stool may appear clay-colored to colorless, while the urine is dark in color. Often this occurs with cholestatic jaundice and hepatitis.
- Fatigue, exhaustion, loss of performance are among the uncharacteristic complaints associated with many liver diseases.
- Loss of appetite, unwanted weight loss.
- Ascites: Increasing waist size with liver cirrhosis or liver weakness.
- Edema in the legs suggests right heart failure.
- Fever is noticeable in acute inflammatory diseases, such as viral hepatitis and inflammation of the pancreas or gallbladder.
- Fatty stool usually occurs as a result of biliary diseases such as gallstones (cholelithiasis).
- Clouding of consciousness, confusion and disorientation can occur in the end-stage of liver cirrhosis or in liver failure. These symptoms lead to what is known as a hepatic coma.
- Strong bad breath. However, this only occurs with acute liver failure.
Note: Jaundice with no pain and accompanying symptoms may indicate an underlying cancer. Be sure to have this clarified by a doctor.
Diagnosis of jaundice
In a personal conversation to collect your medical history (anamnesis), the doctor will first ask you questions about your lifestyle, your medication consumption, your eating habits and any previous illnesses.
Information about stays abroad or pregnancy can also help to track down the cause of jaundice. You should also speak openly about your alcohol consumption. Because from this the doctor can draw important conclusions about the condition of your liver.
Also tell the doctor exactly how long the symptoms have been present, whether you are in pain and whether other symptoms accompany the yellowing.
During the subsequent physical examination, the doctor palpates the liver and bile through the abdominal wall.
If, for example, he finds that the surface of the liver is small, firm and knotty, this indicates cirrhosis of the liver.
In the case of diseases of the gallbladder, it can only be felt painfully. Feeling the spleen may indicate an increased breakdown of blood.
Blood tests are also useful for jaundice:
- If the bilirubin is increased to values above 2 mg / dl (milligrams per deciliter), this is noticeable through yellow eyes.
- Elevated levels of glutamate pyruvate transaminase (GPT) indicate liver damage.
- Glutamate oxalate transaminase (GOT) can be increased in inflammation of the liver and biliary diseases, but also in the event of a heart attack. Chronic alcohol abuse is also reflected in increased values.
- Gamma-glutamyl-transferase (Gamma-GT) is a specific liver enzyme. An increased reading can be caused, for example, by chronic alcohol consumption.
- There are also blood values of the pancreas such as alpha-amylase, which is increased in inflammation.
Imaging procedures round off the diagnosis. With the ultrasound (abdominal sonography) the organs of the abdominal cavity can be visualized quickly and painlessly.
In this way, the doctor can easily assess changes in the surface and size of the liver, but also of the gall bladder and the heart.
More complex imaging such as magnetic resonance imaging (MRI) or computed tomography (CT) is more likely to be used when cancer is suspected.
Taking a tissue sample (biopsy) can provide complete certainty. A small surgical procedure is necessary for this.
Note: Once the doctor has found the cause of the jaundice, he will initiate appropriate treatment.
Important investigations
These examinations help to find out the causes of the symptoms:
- biopsy
- Blood test
- ERCP
- Magnetic resonance imaging
Prevention of jaundice
What Can You Do By Yourself?
If the jaundice is noticeable through yellow eyes or a yellowish skin color, only going to the doctor will help. It is important to uncover the cause and to treat the jaundice properly. There are no home remedies or other methods for jaundice – the only therapy is treatment of the underlying disease.
However, there are a few things you can do to try to prevent jaundice :
- Change your diet: Gallstones, fatty liver and pancreatitis are the consequences of an unhealthy, high-fat diet. Such a diet is often associated with slightly overweight and is harmful to the heart and blood vessels. Therefore, pay attention to a healthy, balanced, low-fat menu.
- Protect against hepatitis: With the vaccination against hepatitis A and B, you can eliminate two dangers at once.
- Travel Smart: Familiarize yourself with the customs and dangers of your travel destination, especially if it is a hepatitis risk area. Inadequate hygiene means that the hepatitis virus is transmitted particularly quickly via contaminated food. But you should also be careful of mosquitoes and tropical diseases. Take into account the country-specific vaccination recommendations. Your family doctor can advise you on this.
- Enjoy alcohol in moderation: For healthy women, a standard glass of alcohol a day (e.g. a glass of wine or a small beer) is considered to be low-risk. In healthy men, double the amount is medically acceptable.