Lyme disease is the umbrella term for a group of bacterial infectious diseases. Borrelia are the trigger. This group mainly includes relapsing fever and Lyme disease. However, the term Lyme disease is often equated with Lyme disease: it is the only disease caused by Borrelia native to Europe. Here you can find out everything you need to know about the routes of infection, symptoms and treatment of rash with Lyme disease.
ICD codes for this disease: M01 | G01 | A68
Quick overview
• What is Lyme disease? Bacterial infection transmitted by tick bites, mostly in the warm season. Incubation period: days, weeks and months elapse between the sting and the onset of the first symptoms.
• Distribution: Everywhere in forested and plant-populated Europe and North America.
• Symptoms: flat, often round skin reddening, flu-like symptoms with headache, body aches, fever; Paraesthesia, paralysis, nerve pain in neuroborreliosis; inflammation of the joints (Lyme arthritis); Heart muscle inflammation (Lyme carditis).
• Diagnostics: Evidence of blood and/or cerebrospinal fluid tests (liquor test); more rarely samples from joint and skin.
• Treatment: with antibiotics for several weeks.
• Prevention: Skin inspection after all outdoor activities, early and professional removal of the tick.
Rash with lyme disease: description
Lyme diseases are caused by mobile, screw-shaped bacteria: the Borrelia. They infest humans and other mammals. Blood-sucking insects serve as carriers. The bacteria can only get into the skin of other living beings through the bites of these parasites.
In most cases, Lyme disease is transmitted to us by a tick bite (not a tick bite), namely by the bite of the common wood beetle (Ixodes ricinus). Occasionally, living beings also become infected through other bloodsuckers such as horseflies, mosquitoes or fleas. There is no direct infection from person to person.
The most common Borrelia disease in humans is rash with Lyme disease. It occurs almost worldwide in temperate climate zones and thus also in our latitudes. In the tropics and subtropics other forms of Borrelia diseases are also widespread, such as lice or tick relapsing fever. It is rarely brought to Germany by travelers or refugees.
Rash with lyme disease
Lyme disease is the most common tick-borne disease in Europe. It is triggered by certain closely related Borrelia, all of which belong to the species complex Borrelia burgdorferi sensu lato (Bbsl).
How many ticks in an area are infected with Lyme disease pathogens varies greatly on a small scale – the infection rate fluctuates between five and 35 percent. And not always when an infected tick bites a person, it transmits Borrelia. Even after transmission, only a small proportion of those infected actually develop Lyme disease (a good one percent).
The prognosis for patients depends to a large extent on rapid treatment: early detection and treatment of Lyme disease usually heals completely. Under certain circumstances, however, the disease can lead to serious complications, secondary diseases and long-term damage.
Lyme disease: occurrence
There are no typical Lyme disease areas, as is known, for example, from TBE (tick-borne encephalitis). Rash with Lyme disease occurs in all wooded and plant-covered areas in Europe and North America.
Since ticks cause Lyme disease in humans, there is a seasonal accumulation of the disease – ticks are dependent on warm weather (the common wood tick becomes active from around 6°C). This means that you can get infected with Lyme disease between April and October in this country in particular (earlier or later in the year in warm weather). Most infections occur in the summer months.
Lyme disease: incubation period
As a rule, days to weeks pass between the tick bite and the appearance of the first symptoms of Lyme disease. “Incubation period” is what physicians call this period of time between infection and the outbreak of the disease.
About half of those affected develop a typical reddening of the skin called “reddening”, medically called erythema migrans. Their incubation period averages seven to ten days. In infected people who do not develop a “migratory blush”, the disease often only becomes noticeable weeks after infection with general symptoms such as exhaustion, swollen lymph nodes and a slight fever.
There are also patients who only show signs of organ involvement weeks to months, sometimes even years after infection. These include skin changes (acrodermatitis chronica atrophicans) or painful joint inflammation (Lyme arthritis).
Signs of Lyme disease in the nervous system (neuroborreliosis) or the heart (Lyme carditis) usually only appear a few weeks after the infectious tick bite.
Because the incubation period for Lyme disease can also be relatively long, some patients can no longer remember the tick bite. Often this was not even noticed.
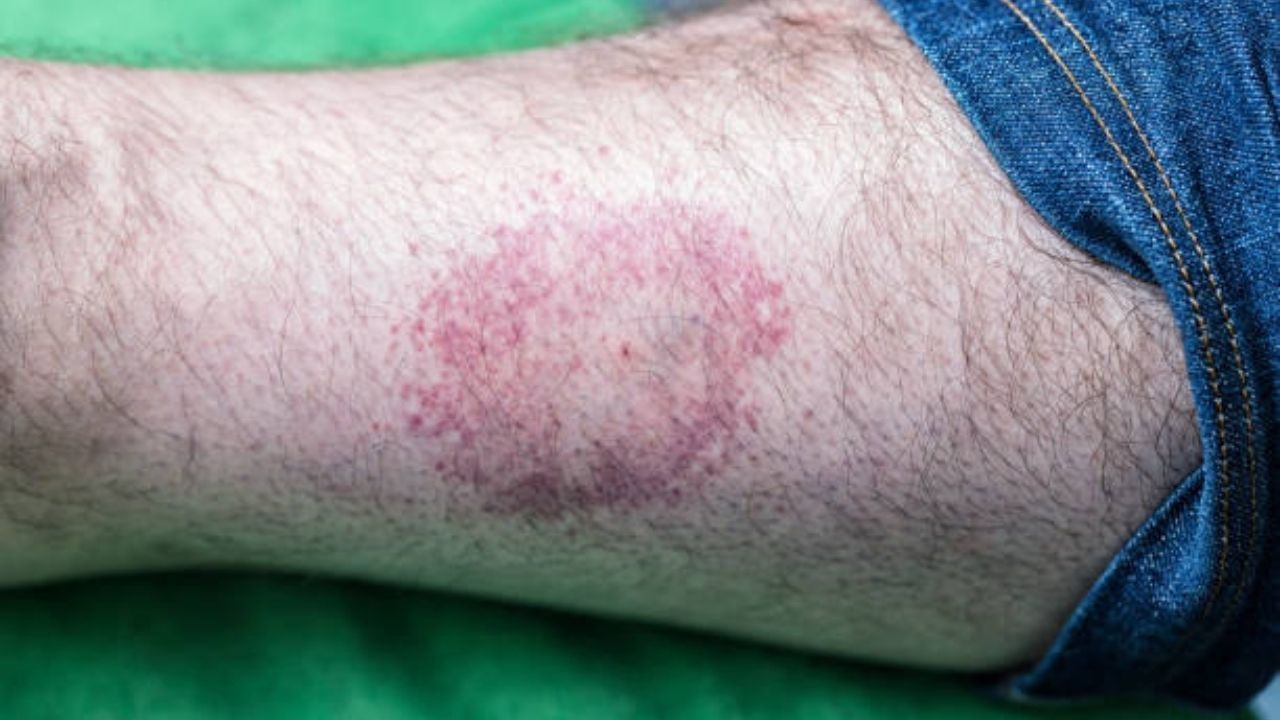
Symptoms of lyme disease
Lyme disease can manifest itself in many ways. Many people with Lyme disease initially show no symptoms at all. In others, reddening of the skin develops at the puncture site, which gradually increases in size. Physicians speak here of erythema migrans, the “migratory blush”. Accompanying flu-like symptoms can occur, such as headaches and body aches as well as fever.
After a tick bite, the Borrelia spread in the tissue. Under certain circumstances, they then spread through the blood in the body and infect different organs. In this way, reddening of the skin also occurs elsewhere.
In some cases, the infection spreads to the nervous system. Then a neuroborreliosis develops (see below). Less frequently, the Borrelia affect other body organs such as the heart.
Long-term effects include chronically inflamed, painful and swollen joints (Lyme arthritis) or progressive skin changes (acrodermatitis chronica atrophicans).
Neuroborreliosis
Neuroborreliosis develops when Borrelia infects the nervous system. The nerve roots of the spinal cord often become inflamed (radiculitis), causing excruciating, burning nerve pain. They are especially noticeable at night.
In addition, neuroborreliosis can be accompanied by flaccid paralysis (e.g. in the face) and neurological deficits (sensory disturbances on the skin). Children in particular often suffer from meningitis.
Neuroborreliosis is usually curable. In severe cases, however, damage can remain. Very rarely, neuroborreliosis takes a chronic course, with the central nervous system (brain, spinal cord) typically becoming inflamed. Those affected are increasingly suffering from gait and bladder disorders.
Causes and risk factors of lyme disease
The causative agents of Lyme disease are bacteria from the species group Borrelia burgdorferi sensu lato. Ticks transmit these Borrelia to humans. There is no direct infection from person to person. That’s why nobody with Lyme disease is contagious! Or to put it another way: sick people are not contagious !
Ticks transmit Lyme disease pathogens
The older a tick is, the higher the risk that it carries Lyme disease pathogens. The tick first has to infect itself with the bacteria: it infects small rodents and other forest dwellers that carry Borrelia. The bacteria do not make the tick sick themselves, but survive in their gastrointestinal tract.
Ticks live especially on grass, leaves and in bushes. From there, she can grab onto passing people (or an animal) in a flash. It then migrates to warm, moist, and dark areas of the body to suck blood. The armpits and the pubic region, for example, are particularly popular. However, ticks can also attach themselves to any other part of the body.
Does Lyme disease infection occur immediately?
While a tick sucks blood from a person, it can transmit Borrelia. However, this does not happen immediately, but only after several hours of vacuuming. The Borrelia are in the gut of the tick. As soon as the tick begins to suck, the bacteria migrate to the salivary glands of the tick and then enter the body of the bitten person with the saliva.
A lower time limit for the act of sucking, from which a Borreliosis infection can be expected, cannot be reliably specified – also because the probability of Borrelia transmission varies depending on the Borrelia species. In general, it is assumed that the risk of Lyme disease is low if an infected tick has been sucking on a human for less than 24 hours. If the blood meal lasts longer, the risk of Lyme disease transmission increases.
Examinations and diagnosis of lyme disease
Tick bite – yes or no? The answer to this question is an important clue for the doctor. However, since the first symptoms of Lyme disease often only appear weeks or months after infection, many patients no longer remember the tick bite or did not even notice it. You can then at least tell the doctor whether there was a chance: Anyone who often goes for walks in forests or meadows or pulls weeds in the garden can easily catch a tick.
In addition to the possibility of a tick bite, the doctor is also interested in the exact symptoms of the patient: the ” reddening ” is particularly meaningful in the early stages of the disease . You should also inform the doctor about general symptoms such as headaches and body aches. In later stages of the disease, patients often report persistent joint problems or nerve pain.
The suspicion of “borreliosis” can finally be substantiated by laboratory tests. The doctor can look for antibodies against Borrelia in a blood or cerebrospinal fluid sample (in the case of neuroborreliosis). However, the interpretation of such laboratory results is not always easy.
Treatment of lyme disease
Like other bacteria, Borrelia can be fought with antibiotics. The type, dose and duration of use of the medication depend primarily on the stage of the Lyme disease and the age of the patient. Adults in the early stages of the disease are usually given tablets containing the active ingredient doxycycline. However, this antibiotic must not be used in children under the age of nine (i.e. before the end of tooth enamel formation) and pregnant women. Instead, the doctor prescribes amoxicillin here, for example.
In later stages of the disease (chronic neuroborreliosis, etc.), doctors often also use antibiotics such as ceftriaxone or cefotaxime. The medication is usually given as a tablet, but sometimes also as an infusion through a vein (eg ceftriaxone).
The success of antibiotic therapy depends in particular on the start of treatment: In the early stages of rash with lyme disease, the treatment is usually more effective than in later stages.
Lyme disease: course of the disease and prognosis
The rapid start of therapy is very important in Lyme disease. The course and prognosis of the disease are significantly influenced by whether the bacteria have had time to spread and multiply in the body. With the right treatment, the symptoms usually disappear completely.
Under certain circumstances, signs of Lyme disease also persist. Sometimes patients retain mild facial nerve palsies for life. Other sufferers have protracted joint pain. A reaction of the immune system that lasts beyond the infection causes inflammation here.
Early signs are often missing or go unnoticed, which is why Lyme disease is recognized and treated later. The treatment of Lyme disease in such advanced stages of the disease is always difficult. Sometimes an additional course of antibiotics is required.
The experts in the medical guidelines do not recommend antibiotic therapies that last for months, multiple repetitions or combinations of several active ingredients!
In some cases, people become infected without developing clear signs of illness afterwards. Antibodies against Borrelia can be detected in about every fifth German over the age of 70 – in most cases without previous illness. The infection therefore heals itself and with the help of the immune system.
However, once Lyme disease has been overcome, which has healed spontaneously or under therapy, does not offer any immunity. This means that you can later become infected with Lyme disease and fall ill with it.
Post-Lyme Disease Syndrome
Post-borreliosis syndrome is particularly popular in health magazines and the media. However, there is no clear definition that describes this clinical picture. The media report on patients who complain, for example, of muscle pain, tiredness, lack of drive or lack of concentration.
However, previous studies indicate that these non-specific symptoms in people who have had a Borrelia infection do not occur more frequently than is generally the case. Many experts therefore doubt that the supposed “post-borreliosis syndrome” is actually related to borreliosis.
Known late effects of a Borrelia infection are persistent skin changes (acrodermatitis chronica atrophicans), joint inflammation (Lyme arthritis) or neurological symptoms (chronic or late neuroborreliosis).
If those affected suffer from post-Lyme disease symptoms, it is advisable to clarify other possible causes of these symptoms. For example, the reason for chronic fatigue or lack of concentration can be a viral infection or even hidden depression. The doctor can then initiate appropriate treatment.
Lyme disease & pregnancy
Earlier case reports and small studies initially suggested that Borrelia infection during pregnancy disrupted child development. However, more recent studies have not yet confirmed this assumption.
However, there is no evidence that unequivocally rules out the harmful effects of an infection during pregnancy. That is why the doctor treats Lyme disease during pregnancy consistently with antibiotics. To do this, he chooses active ingredients that do not harm the mother or the unborn child.
According to the current state of knowledge, women who have already had Lyme disease and were treated accordingly before becoming pregnant do not have to worry.
In addition, there is no evidence that mothers can transmit Lyme disease through breastfeeding.
Prevention of lyme disease
Ticks offer the only starting point for protection against Lyme disease: Prevent tick bites or remove a tick that is already sucking as quickly as possible. The following tips apply for this:
If you are out and about in the woods and meadows or doing gardening, you should wear light-colored (white) clothing if possible. Ticks are easier to spot on them than on dark textiles. The arms and legs should also be covered by clothing so that the little bloodsuckers do not come into contact with skin so easily.
You can also apply tick or insect repellents. However, keep in mind that these do not offer 100% protection against a tick bite and are only effective for a few hours.
Avoid taking shortcuts through tall grass and bushes. Instead, stay on paved trails.
In any case, you should thoroughly check your whole body for ticks after spending time outdoors. Also check your pets for possible ticks: the parasites could pass from your cat or dog to you.
If you find a sucking tick on your skin, you should remove it immediately and professionally : grasp the tick with fine tweezers or tick tweezers just above the skin and pull it out slowly and without twisting. Press as little as possible to avoid squeezing the animal’s bodily fluids into the wound. Also check that you have not accidentally ripped off the body while the parasite’s head is still in the wound.
If you try to poison or suffocate a tick sucking on the skin with oil or other substances, you increase the risk of infection! Because in the struggle for survival, the tick may transmit even more Borrelia.
You should then disinfect the puncture wound. This does not protect against Lyme disease, but prevents wound infection.
Taking antibiotics as a precaution after a tick bite (without a diagnosis of Lyme disease infection) is not recommended.
There is no Lyme vaccine!
Doctors can vaccinate against tick-borne encephalitis (TBE), which is also transmitted by ticks. It is particularly advisable for those who live in or travel to risk areas. However, there is no preventive vaccine against Lyme disease.
