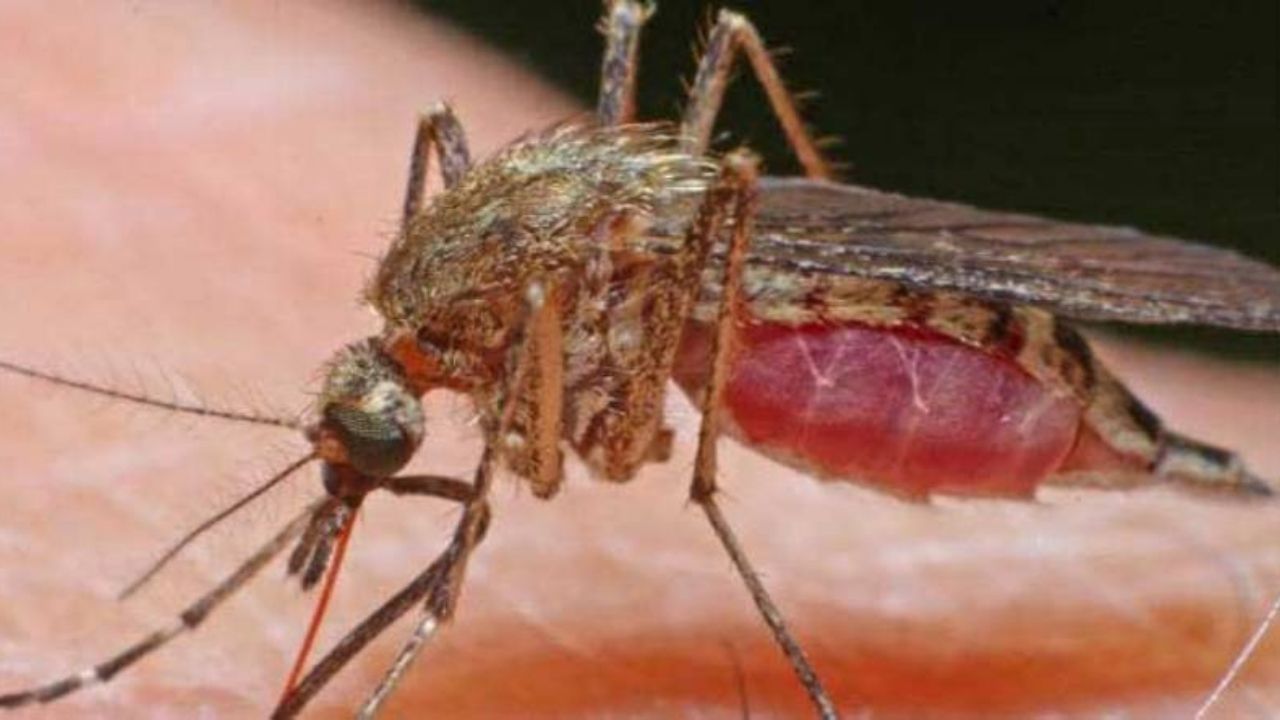
The Japanese encephalitis is the Asian region’s the most important viral infection of the brain. It is caused by the Japanese encephalitis virus, which is transmitted by mosquitoes. It mainly affects locals (especially children).
Most of the time the disease is only mild. But it can also lead to permanent damage or death. Read more about Japanese encephalitis, its symptoms and treatment here.
Overview
- What is Japanese encephalitis? A virus-related encephalitis that is particularly common in Southeast Asia.
- Causes : Japanese encephalitis viruses, which are transmitted by blood-sucking mosquitoes
- Symptoms : mostly no or only mild symptoms such as headache and fever, in children mainly gastrointestinal complaints. Rarely severe courses with symptoms such as high fever, stiff neck, seizures, paralysis, impaired consciousness and even coma.
- Diagnosis : Detection of specific antibodies against the Japanese encephalitis virus in the blood or nerve fluid.
- Treatment : only possible symptomatically (alleviation of symptoms); if necessary intensive medical care.
- Forecast : 1 in 250 infected people will become seriously ill. Up to 30 percent of those affected die. 20 to 30 percent of the survivors suffer permanent consequential damage (such as paralysis).
Japanese encephalitis: description
Japanese encephalitis is inflammation of the brain caused by a virus. A risk of infection exists mainly in Southeast Asia and the western Pacific region and thus for more than three billion people.
An infection with the Japanese encephalitis virus only rarely leads to a manifest disease (i.e. the outbreak of symptoms). But if it does, the death rate is high.
According to the World Health Organization (WHO), an estimated 68,000 people worldwide develop Japanese encephalitis every year. The disease leads to death in 13,600 to 20,400 patients annually.
Japanese Encephalitis: Occurrence and Risk Areas
The risk areas for infection with Japanese encephalitis range from East Asia (e.g. East Siberia, Korea, Japan) to Southeast Asia (Thailand, Vietnam, Cambodia, Philippines, Indonesia etc.) to South Asia (India, Nepal etc.). In the western Pacific, for example, you can also get infected with the Japanese encephalitis virus in Papua New Guinea. And the viral disease even occurs on the northern tip of Australia.
In the temperate climatic zone of Asia, you can get infected with Japanese encephalitis, especially in summer and autumn. In tropical-subtropical regions there is the greatest risk of infection during and after the rainy season. Basically you can get infected with the pathogens of Japanese encephalitis in these areas all year round.
Symptoms of japanese encephalitis

Four to 14 days (incubation period) elapse between infection and the appearance of the first symptoms. However, most infected people develop no symptoms at all or only mild symptoms that are similar to those of a flu-like infection (such as fever and headache). In children with Japanese encephalitis, abdominal pain and vomiting can be the main initial symptoms.
After two to three days of flu-like symptoms, the condition of those affected may suddenly worsen. But that rarely happens: only one in 250 infected people becomes seriously ill with Japanese encephalitis. Symptoms are then:
- High fever
- A headache
- Stiff neck
- Photosensitivity
- Disorder of movement coordination (ataxia)
- Tremor
- Disturbances in consciousness up to coma
- Seizures
- spastic paralysis
These severe symptoms of Japanese encephalitis can be explained by the spread of the infection to the central nervous system: encephalitis develops, which can subsequently also spread to the meninges (combined meninges and meningitis = meningoencephalitis). Additional inflammation of the spinal cord is also possible (meningomyeloencephalitis).
Such a severe course of Japanese encephalitis is often fatal or has neurological and psychiatric consequences. These include, for example, symptoms of paralysis, repeated seizures or the loss of language skills.
Japanese encephalitis is often severe, especially in young children and the elderly.
Causes and risk factors of japanese encephalitis
Japanese encephalitis is caused by the Japanese encephalitis virus (JEV). It belongs to the so-called flaviviruses. Other representatives of this virus family are, for example, the West Nile virus, the yellow fever virus and the causative agent of early summer meningoencephalitis.
The Japanese encephalitis virus is found primarily in domestic pigs and water birds. In these animals, the pathogen is often highly concentrated in the blood. This does not cause any disease in the animals. However, mosquitoes of the genus Culex (especially Culex tritaeniorrhynchus, the rice field mosquito) can ingest the virus when they suckle blood from these animals. If the mosquito infected in this way then bites a person, they in turn can become infected.
In contrast to infected pigs or water birds, the amount of virus in the blood of infected people can never rise so high that healthy mosquitoes become infected during a blood meal and thus become a risk of infection for other people.
There is an increased risk of contracting Japanese encephalitis, especially for the population in rural and urban areas in the above-mentioned risk regions. There people usually live in closer proximity to the host animals of the pathogen (pigs, water birds).
Japanese encephalitis is particularly common in regions with extensive rice cultivation and / or pig breeding. Rice-growing areas play a role because the moist environment offers optimal breeding conditions for the main carriers of the disease – the rice field mosquitoes.
The humidity is also the reason why disease outbreaks often increase during the rainy season and afterwards – many stagnant bodies of water in combination with a warm climate offer ideal conditions for the spread of the Japanese encephalitis virus.
Diagnosis of japanese encephalitis
If someone lives or has traveled to one of the risk areas above and develops signs of inflammation of the brain (encephalitis), the cause is likely to be the Japanese encephalitis virus. For clarification, the WHO recommends an antibody test: In the patient’s blood or – even better – nerve fluid (liquor), a search should be made for specific IgM antibodies against the pathogen. If they can be detected, this speaks for Japanese encephalitis.
At the same time, other possible causes of the brain inflammation (e.g. other viruses, bacteria) must be ruled out with suitable examinations. This prevents other, treatable causes such as bacterial infections from being overlooked.
Treatment of japanese encephalitis
So far there is no specific, i.e. causal therapy for Japanese encephalitis. The disease can only be treated symptomatically, i.e. by alleviating the patient’s symptoms. For example, the doctor can give the patient anticonvulsants.
Treatment for Japanese encephalitis is often done in the intensive care unit. If necessary, a poor general condition can be better stabilized there. In particular, intracranial pressure must be carefully monitored and possibly reduced (encephalitis can cause the brain to swell dangerously!).
Japanese encephalitis should be treated as quickly and carefully as possible. This increases the patient’s chances of survival and lowers the risk of consequential damage.
Japanese encephalitis: disease course and prognosis
Even if a Japanese encephalitis infection is usually asymptomatic or only mild, it should be taken seriously. After initially mild symptoms, it can suddenly turn into a severe course by triggering inflammation in the central nervous system. As a result, up to 30 percent of those affected die. Of those who survive the disease, 20 to 30 percent suffer from permanent consequences. This includes intellectual, behavioral and neurological damage.
Vaccination of japanese encephalitis
Anyone planning a trip to an area where Japanese encephalitis is spread can protect themselves from infection with a vaccination. The available vaccine can be injected from the age of 2 months. Two vaccination doses are necessary for effective vaccination protection. They are usually given 28 days apart.
For adults up to 65 years of age there is also the option of a faster vaccination schedule, for example when traveling to Asia on short notice. The second dose of vaccine is given 7 days after the first dose.
Japanese Encephalitis: Other Preventive Measures
In addition to vaccination, there is another way to prevent infection with the Japanese encephalitis virus – through careful protection against mosquito bites:
The Culex mosquitoes, which transmit the Japanese encephalitis virus, are mostly active in the evening and night. During this time you should be particularly careful to protect yourself from mosquito bites if you are in a risk area. Important tips:
- Wear long sleeved clothing and long pants. The less your skin is exposed, the less chance mosquitoes have to settle on you for a meal of blood.
- Use a suitable mosquito repellent.
- Sleep under a mosquito net that will keep the carriers of Japanese encephalitis away from you at night.