Hand, foot and mouth disease (HFMD) is a mostly harmless but highly contagious viral disease. Children in particular are affected. The disease is transmitted through bodily fluids, stool, or contaminated objects. Typical symptoms are painful blisters on the hands and feet and in the mouth area. Hand, foot and mouth disease usually heals after ten days at the latest without any consequences. Read everything you need to know about symptoms, causes, diagnosis, treatment and possible complications here.
ICD codes for HFMD : B08
Quick overview
- Symptoms: First flu-like symptoms, then red spots and blistering on the hands, feet and mouth; the infection is often asymptomatic
- Course and prognosis: In most cases heals by itself and without complications, complications rarely develop due to the infection spreading to internal organs (e.g. meningitis)
- Causes: Smear or droplet infection with certain viruses (enteroviruses), which occur everywhere in the environment and are highly contagious
- Diagnostics: Often based on the typical symptoms and the information from the anamnesis interview, in severe or unclear cases further examinations (blood, stool)
- Treatment: Relief of symptoms with painkilling tinctures, calf wraps to reduce fever, etc.
What is hand, foot and mouth disease?
Hand, foot and mouth disease (HFMD) is a generally harmless but highly contagious viral infection that primarily affects children under the age of ten. The triggers of hand, foot and mouth disease, various enteroviruses, are ubiquitous in the environment and are highly contagious. You never really get any peace from hand, foot and mouth disease: it occurs all year round, with a peak in late summer and autumn.
Infection
The disease is transmitted from person to person : This happens, for example, directly via bodily fluids such as nasal and throat secretions, saliva or secretions from the typical skin blisters. For example, when infected people cough or sneeze, they spread tiny droplets of saliva around them, which transmit the pathogen to healthy people (droplet infection). Infection is also possible when touching the blister secretion.
In addition, hand, foot and mouth disease can be transmitted via smear infection : the secretion droplets containing the virus contaminate objects and surfaces such as cutlery or doorknobs, which then become a source of infection for healthy people. In addition, infected people excrete the virus in their stool. If they don’t wash their hands (properly) after a bowel movement, they may contaminate faucets, doorknobs and other objects in the process.
The incubation period of HFMD, i.e. the time between infection and the appearance of the first symptoms, is three to ten days on average. However, sometimes the infection becomes noticeable even before that (at the earliest one day after infection) or much later (up to a month later).
Duration of the risk of infection
Those affected are most contagious in the first week of the illness. In this phase, the viruses multiply particularly quickly, so that large numbers of them enter the environment via body fluids and stool.
However, there is still a certain risk of infection even after the symptoms of hand, foot and mouth disease have subsided: In some cases, infected people continue to excrete the pathogens in their stool for weeks. It is therefore generally advisable to wash your hands thoroughly after going to the toilet or changing diapers.
Many infected people (especially adults) show no symptoms of the disease. But they are still contagious!
What are the symptoms of early-stage HFMD?
The term “hand, foot and mouth disease” already gives an idea of the parts of the body where the characteristic symptoms of the disease appear. Initially, however, it manifests itself in non-specific, flu-like symptoms such as fever, poor performance, sore throat and body aches, and loss of appetite.
Typical symptoms later on
About a day or two later, painful red dots develop in the mouth (tongue, gums, oral mucosa) and around the mouth (perioral) , which soon become small blisters or superficial ulcers (aphthae).
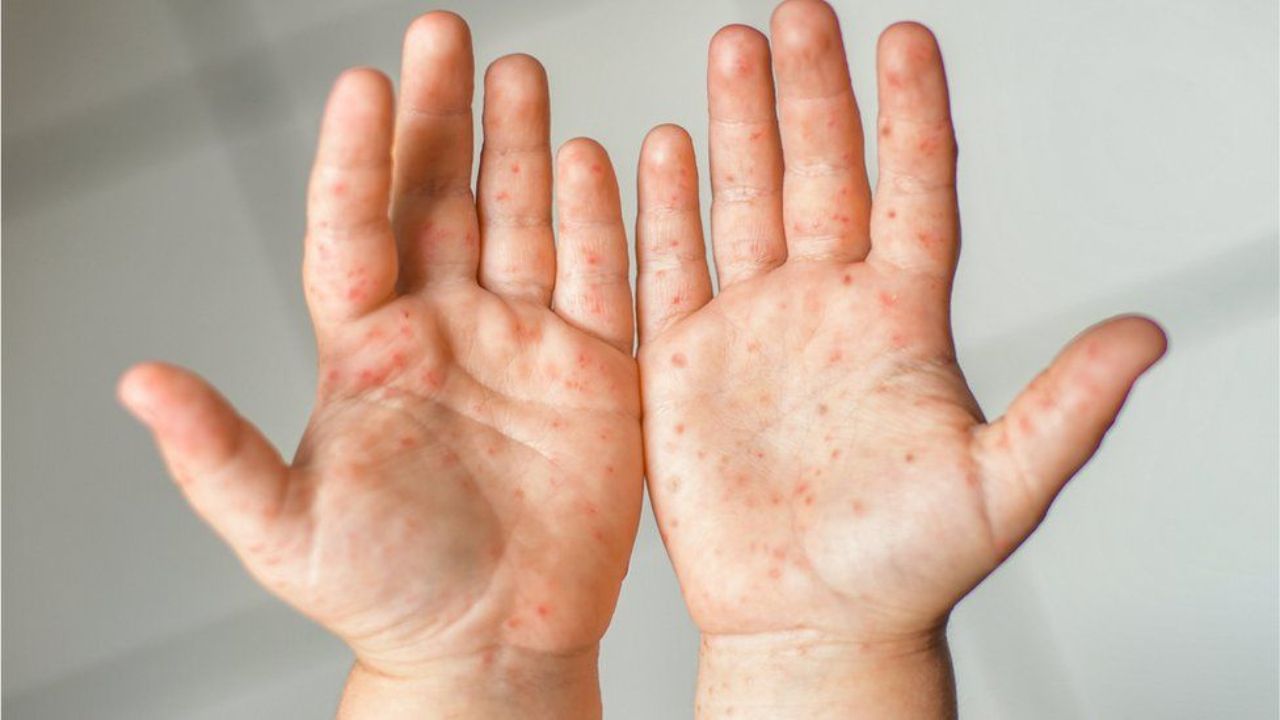
A rash develops on the hands and feet at about the same time as the red spots in the mouth or a few hours later : it usually appears as many red spots of different shapes and sizes, which are usually not itchy at first. However, this may change if blisters form on the reddened areas. Typically, the palms of the hands and soles of the feet are affected by this rash. Sometimes it also develops in other places such as the backs of the hands, buttocks, genitals, knees or elbows.
Some sufferers lose their fingernails and toenails about four to eight weeks after the disease has subsided.
The skin blisters in hand, foot and mouth disease secrete a secretion that contains many of the causative viruses. As a result, the patient transmits the virus to other parts of his body and – by touching objects – to other people. Thorough hygiene is therefore very important during the illness!
Non-symptomatic courses
For many sufferers, hand, foot and mouth disease causes no symptoms at all. Doctors assume that the symptoms described only occur in four out of five infected people. The symptoms of hand, foot and mouth disease are often very mild, especially in adults. As a result, they often do not even notice the infection. The same applies to children over the age of ten. However, even in this case there is a risk of infection for others.
So if you suspect you have the disease, for example because you notice individual (non-specific) symptoms, you should try not to be in the presence of small children during the time of the disease.
What is hand, foot and mouth disease in adults?
Hand, foot and mouth disease usually goes away on its own after seven to ten days without any complications. Especially in adults, the course of the disease is usually very mild, often even asymptomatic. In people with a weakened immune system, complications with severe disease courses may develop if the virus spreads in the body. Possible consequences are, for example, meningitis or damage to the heart or liver.
Hand, foot and mouth disease in pregnancy
If a pregnant woman becomes infected with hand, foot and mouth disease, there is generally no reason to worry: the infection is usually very mild or has no symptoms at all, even during pregnancy. However, if the pregnant woman develops symptoms of hand, foot, and mouth disease shortly before or after delivery, there is a chance that she may pass the infection on to the newborn.
Course in newborns, infants and children
Newborns and infants are particularly at risk of complications. In them, the disease sometimes spreads to organs such as the liver and heart, which can lead to very severe courses. This risk is highest in newborns in the first two weeks of life. Complications are very rare in older children, and the disease usually heals without consequences.
Due to the high risk of infection, sick children should not visit community facilities such as day care centers and schools until the symptoms have completely subsided. The same applies to siblings if they also show possible signs of hand, foot and mouth disease.
Once you have had the disease, you are immune to the specific type of virus that causes it. However, if you contract hand-foot-and-mouth disease from another type of virus, it is possible to get the disease again.
Causes and risk factors
Various enteroviruses are responsible for the disease, most notably Coxsackie A viruses and enterovirus A71. They are widespread, and if someone falls ill in a day care center, kindergarten or school, it usually doesn’t take long for the highly contagious disease to spread.
Even adults are not protected from hand, foot and mouth disease. People with a weakened immune system are particularly at risk. The cause of such an immune deficiency is, for example, other diseases (such as HIV) or an immune-weakening therapy. Due to the weakened immune system, the pathogens of hand, foot and mouth disease cause meningitis or damage organs such as the liver and heart in the worst case.
Hand, foot and mouth disease is often mistakenly referred to as foot and mouth disease. However, this disease only occurs in cattle, sheep and pigs and is unrelated to hand, foot and mouth disease. Nevertheless, the latter is often called “false foot-and-mouth disease”.
Hand, Foot, and Mouth Disease: Examinations & Diagnosis

If you suspect hand, foot and mouth disease in yourself or in your child, the family doctor or pediatrician is the right person to talk to. He will first obtain all relevant information on the medical history in the interview. For example, the doctor asks:
- What symptoms have occurred (fever, sore throat, loss of appetite, rash, etc.)
- Whether there was contact with other children/adults with hand, foot and mouth disease
- Whether the patient is taking medication
- What diseases are vaccinated against?
The background to the last question is that rashes also occur with other typical “teething troubles”. If you have been vaccinated against it, such diseases can be ruled out as the cause of the symptoms with a high degree of certainty.
After the anamnesis interview, a physical examination follows. Among other things, the doctor looks at where a rash has formed and what it looks like.
Hand, foot and mouth disease can usually be clearly diagnosed based on the information from the anamnesis interview and the physical examination. Further examinations are usually only necessary if the clinical picture is very severe or the symptoms cannot be unequivocally assigned to hand, foot and mouth disease. For further clarification, the doctor then examines a blood or stool sample, for example. Rarely, he takes a sample of the cerebrospinal fluid (liquor puncture) and sends it to the laboratory for analysis.
There are some diseases that cause symptoms similar to hand, foot and mouth disease in the mouth. These include tonsillitis, glandular fever and herpes.
Treatment
Hand, foot and mouth disease cannot be treated causally, which means that there are no medications available to combat the virus that causes it. However, this is not necessary because the disease is usually harmless. Treatment is limited to relieving the symptoms, for example with a pain-relieving and fever-reducing drug (for example with the active ingredient paracetamol).
Acetylsalicylic acid (ASA) is also a popular painkiller and antipyretic. However, it is not suitable for children: In some cases, the drug, in combination with a viral infection, causes serious complications such as Reye’s syndrome.
Doctors may prescribe a mild, pain- relieving tincture for dabbing or rinsing on for sore mouth blisters. This usually contains the active ingredients chlorhexidine or lidocaine. Various plant-based remedies (chamomile, lemon balm, thyme) are also said to be able to alleviate symptoms of hand, foot and mouth disease.
Despite the painful blisters in the mouth, those affected should drink enough. Otherwise there is a risk of dehydration, especially in children.
Antibiotics are generally not effective against viral infections because they only help against bacteria. In some cases, however, a bacterial infection (superinfection) develops in addition to the viral hand, foot and mouth disease. Then antibiotic treatment is sometimes necessary.
Hand, foot and mouth disease: home remedies
Not only with conventional medical measures, but also with home remedies, something can be done against the symptoms of hand, foot and mouth disease. Some examples of suitable home remedies :
- Home remedies such as calf wraps can help with fever.
- The blisters in the mouth often make chewing and swallowing painful. Chilled or lukewarm food that does not have to be chewed heavily (such as yoghurt, pudding, soup) and drinks such as cooled camomile or marigold tea are then recommended.
- Patting the painful blisters in your mouth with a cotton swab dipped in honey can help soothe them.
Home remedies have their limits. If the symptoms persist over a longer period of time, do not get better or even get worse, you should always consult a doctor.
Hand, foot and mouth disease: homeopathy
Some people also try to support the healing process of hand, foot and mouth disease with homeopathy. For example, Rhus toxicodendron is said to help against the blister-like rash . Apis and belladonna are generally recommended for feverish infections . An experienced doctor or homeopath can advise you on the selection, use and dosage of homeopathic remedies for hand, foot and mouth disease.
The concept of homeopathy and its specific effectiveness are controversial in science and not clearly proven by studies.
Prevention
There is no vaccination against hand, foot and mouth disease in this country. Extremely thorough hygiene is important to prevent infection or the transmission of the pathogen. This includes washing your hands regularly with soap. This is especially true after sneezing or coughing, after going to the toilet, after changing diapers, and before and after preparing food.
If a family member is ill, potentially contaminated items and surfaces such as doorknobs and toilets should be cleaned with extra care. It is also advisable to avoid close contact with the affected person, such as hugging or kissing. This helps prevent infection with hand, foot and mouth disease.