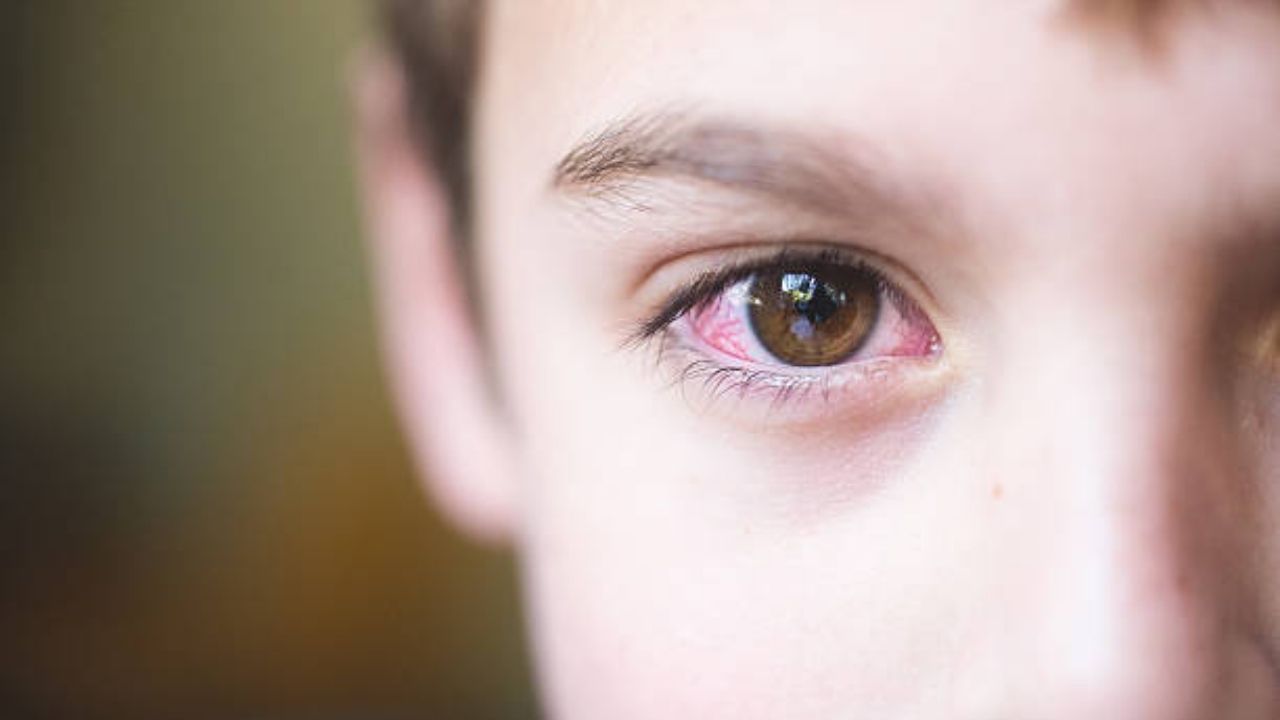
In the case of conjunctivitis, the eye reddens and waters. It often hurts or itches too. Inflammation can be caused by a viral or bacterial infection, an allergy, or an interfering foreign object in the eye. The conjunctivitis therapy looks correspondingly different. Read more about this as well as the causes, symptoms and diagnosis of conjunctivitis here!
Quick overview
- What is conjunctivitis? An infectious or non-infectious inflammation of the conjunctiva. The medical term is conjunctivitis.
- Causes : Infectious agents (such as bacteria, viruses), allergies, foreign bodies in the eye (e.g. dust), damaged contact lenses, UV light, drafts, eyestrain and much more
- Common symptoms : Red, watery and (especially in the morning) sticky eyes, swollen eyelids, swollen conjunctiva, burning and/or itching in the eye, foreign body sensation in the eye
- Treatment : Depending on the cause, eg antibiotics for bacterial conjunctivitis (usually as eye drops); for allergic conjunctivitis (conjunctivitis allergic), anti-allergic eye drops, eye drops containing cortisone if necessary; In general: Eliminate or avoid triggers as far as possible
- Is conjunctivitis contagious? Bacterial and viral conjunctivitis are highly contagious! If you are infected, do not touch your eyes, pay attention to careful hand hygiene and use your own towel.
Symptoms of conjunctivitis
Typical symptoms of conjunctivitis are:
- Red, watery eye.
- Increased secretion from the eye, often resulting in blurred vision and sticky eyes, especially in the morning.
- Swollen eyelid, swollen conjunctiva.
- Photophobia/Sensitivity to glare.
- Foreign body sensation or pressure in the eye.
- Burning and/or itching in the eye.
Depending on the trigger of the conjunctivitis, there may be peculiarities with regard to the symptoms. Examples:
| Type of conjunctivitis | Specific symptoms |
| Bacterial conjunctivitis | – Eye discharge is thick white, green or yellow (purulent)- usually starts in one eye and then spreads to the second within a few days |
| Viral conjunctivitis | – Eye secretion rather watery (serous)- Lymph nodes in front of the ear sometimes swollen and painful- Irritation (irritation) of the affected eye- usually begins in one eye and then rapidly spreads to the second- In the case of systemic viral infections (such as measles, mumps, chickenpox, rubella), corresponding symptoms of the disease are added |
| Allergic conjunctivitis | – The focus is on severe itching |
Causes and risk factors of conjunctivitis
Various types of causes can lead to conjunctivitis. Doctors distinguish between two groups:
- Infectious conjunctivitis : It is caused by bacteria, viruses, fungi or parasites. This form of conjunctivitis is contagious.
- Non-infectious conjunctivitis : This includes all cases of conjunctivitis that are not caused by pathogens but, for example, by allergies or mechanical stimuli.
Below you will find more detailed information on the development of the most important types of conjunctivitis.
Bacterial conjunctivitis
The most common causes of bacterial conjunctivitis are:
- Staphylococcus aureus
- Streptococcus pneumoniae
- Haemophilus species
Sometimes chlamydia (more precisely: Chlamydia trachomatis) are the cause of bacterial conjunctivitis. Doctors then speak of chlamydia conjunctivitis. It can take two forms – trachoma or paratrachoma (“swimming pool conjunctivitis”). Because it is typically associated with a mucopurulent eye secretion, the term mucopurulent conjunctivitis is also used for it.
Another bacterial cause of an inflamed conjunctiva can be bacteria of the Neisseria gonorrhoeae (“gonococci”) type. Then it is gonococcal conjunctivitis.
Both chlamydial and gonococcal infection very often manifest as a venereal disease (called gonorrhea in the case of gonococci). Transmission of the germs into the eyes – either of the infected person or of another person – is possible, for example, if there is a lack of hand hygiene or via (shared) towels.
In addition, pregnant women who are infected with gonococci and/or chlamydia in the genital area can transmit the germs to the newborn at birth, namely during passage through the infected birth canal. As a result, the baby can develop conjunctivitis called neonatal conjunctivitis (or ophthalmia neonatorum).
Bacterial conjunctivitis is usually acute. It can become chronic if it is caused by chlamydia or (more rarely) Moraxella bacteria.
Viral conjunctivitis
Viral conjunctivitis is acute. Sometimes it occurs as part of a cold – caused by cold viruses (such as rhinoviruses) – on. In other (systemic) viral diseases that affect the whole body, the pathogens can also spread to the conjunctiva of the eyes, such as measles, mumps, rubella and chickenpox viruses.
Sometimes, however, the viral infection is limited to the eye (ie does not affect the rest of the body). Such localized viral conjunctivitis is usually caused by adenoviruses, of which there are different types (serotypes). Types 5, 8, 11, 13, 19 and 37 are usually responsible for adenovirus conjunctivitis. It is often difficult. In about a quarter of cases, inflammation of the cornea (keratitis) also develops. Such a simultaneous corneal and conjunctivitis triggered by adenoviruses is called epidemic keratoconjunctivitis.
The above-mentioned chickenpox viruses (varicella-zoster viruses) belong to the herpes virus family. Other members of this virus family can also trigger viral conjunctivitis – the herpes simplex virus (HSV). They are best known as the causative agent of lip and genital herpes, but can also affect the conjunctiva.
This can happen in newborns, for example, if the mother has genital herpes and the child becomes infected around the eyes while passing through the birth canal. However, HSV-related conjunctivitis can also affect small children, older children, adolescents and adults. HSV conjunctivitis often spreads to the cornea of the eye, resulting in keratoconjunctivitis.
A less common cause of viral conjunctivitis is enteroviruses. Acute hemorrhagic conjunctivitis develops here . It is associated with bleeding under the conjunctiva and occurs in Africa and Asia.
Conjunctivitis caused by fungi or parasites
Fungal infections are very rarely the cause of conjunctivitis. Such fungal conjunctivitis can be caused, for example, by Candida or Microsporum fungi or molds of the Aspergillus genus.
Also rarely, the infestation of parasites leads to an inflamed conjunctiva. This can happen, for example, with loa loa – a form of roundworm disease (filariasis). Conjunctivitis can also develop as part of an infection with Leishmania (leishmaniasis) or trypanosomes.
Fungal or parasitic conjunctivitis is more common in tropical-subtropical countries. In the northern hemisphere, it is most likely to occur as an opportunistic infection in an immune system that has been weakened by illness or medication – with a healthy, strong immune system, the pathogens would have little chance.
Allergic conjunctivitis or conjunctivitis allergic
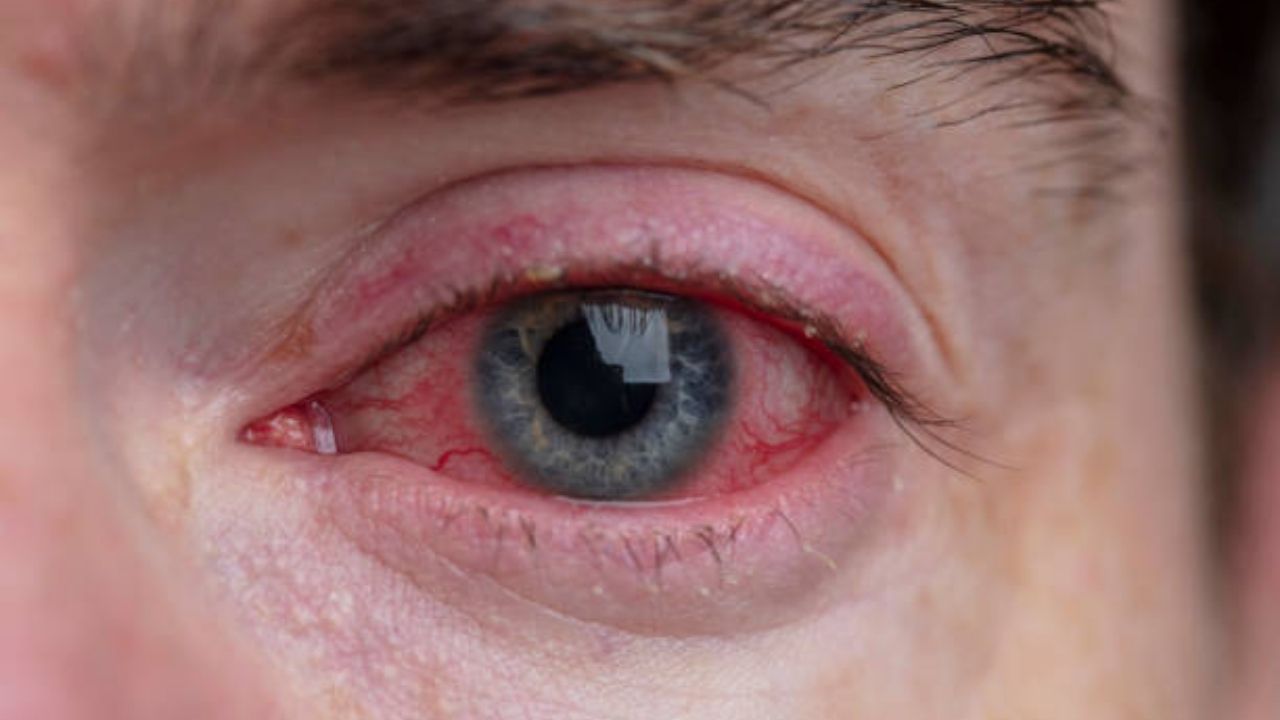
Allergic conjunctivitis or conjunctivitis allergic, is a type I allergic reaction. This means: The hypersensitivity reactions (itchy eyes, tears, etc.) occur within a few minutes or even seconds after contact with the specific allergy trigger (allergen). There are three forms of the disease:
Seasonal allergic conjunctivitis
It is also called hay fever conjunctivitis. This type of conjunctivitis is triggered by mold spores or pollen from trees, grasses or other plants that get into the eye through the air. Depending on the life cycle of the plant in question, seasonal allergic conjunctivitis becomes noticeable mainly in spring, late summer or early autumn.
Atopic conjunctivitis
This form of conjunctivitis is triggered by dust mites (house dust allergy), animal dander (e.g. cat allergy, dog allergy) and other allergens with which those affected can come into contact all year round. If the cornea becomes inflamed in addition to the conjunctiva, this is referred to as atopic keratoconjunctivitis.
Vernal keratoconjunctivitis
This combined corneal and conjunctivitis is most likely of allergic origin and usually occurs in spring. Symptoms subside in autumn and winter. It is most common in male children and adolescents between the ages of five and 20 who suffer from eczema, asthma or a seasonal allergy.
Other types of conjunctivitis
In addition to allergy triggers, there are other possible causes of non-infectious conjunctivitis:
For example, it is often caused by irritation of the eyes by chemical, physical, thermal stimuli or radiation, such as chemical burns or burns to the eyes, make-up, dust, smoke, wind, drafts, wind, cold, UV light (sun, solarium) and welding work. Contact lenses that have been worn too long or are damaged, as well as eyestrain (e.g. due to concentrated near work or lack of sleep) can irritate the conjunctiva so severely that it becomes inflamed.
In other cases, wetting disorders due to reduced tear secretion or altered composition of the tear film are the reason for non-infectious conjunctivitis. The wetting disorder results in dry eyes (keratoconjunctivitis sicca). Possible triggers for this are, for example:
- Extensive screen work (with infrequent blinks)
- Hormonal or metabolic disorders, eg during pregnancy, with estrogen therapy (e.g. during menopause), diabetes mellitus or thyroid diseases
- Certain eye disorders such as dysfunction of the meibomian glands (sebum glands in the eyelid), disorders of the tear ducts or ectropion (opening of the eyelid)
- Certain other medical conditions such as Sjogren’s Syndrome, Rheumatoid Arthritis, Acne, Rosacea
- Medications such as acetylsalicylic acid (ASA), beta blockers or hormonal contraceptives that suppress ovulation (ovulation inhibitors)
Adjacent pathological processes such as a malignant tumor of the Meibomian glands (Meibomian gland carcinoma) can also result in conjunctivitis.
Treatment of conjunctivitis
As with other diseases of the eye, you should always see an ophthalmologist if you have conjunctivitis ! Depending on the cause of the conjunctivitis, he can initiate appropriate treatment and thus prevent permanent eye damage.
Treatment of bacterial conjunctivitis
Bacterial conjunctivitis is treated with antibiotics: ointments or drops containing antibiotics are usually used, which are placed in the eye and act directly at the site of the infection. They are usually used for seven to ten days.
In certain cases of bacterial conjunctivitis, the doctor prescribes antibiotic tablets as an alternative or in addition – for example, necessary for patients in whom a bacterial infection in other parts of the body has spread to the eyes. This can especially happen with a chlamydia infection or a gonococcal infection – two well-known STDs. In such cases, the sexual partner should also be treated with antibiotics so that the couple does not infect each other again.
Even if conjunctivitis symptoms improve before then, it’s important to keep taking antibiotics for as long as your doctor recommends. Otherwise, some bacteria may remain in the body, which multiply again after the treatment is stopped and cause conjunctivitis again.
There are no specifically effective – i.e. antiviral – drugs available for the treatment of viral conjunctivitis. Such come only in viral corneal inflammation for use.
In contrast, treatment for viral conjunctivitis consists of symptom-relieving measures such as cold compresses on the eyes (see: conjunctivitis – home remedies). Artificial tears that are dropped into the eye can also relieve the symptoms.
In the case of severe viral conjunctivitis, eye drops containing corticosteroids (“cortisone” eye drops) can be used for a short period of time to reduce inflammation. In the long term, however, these are not suitable for therapy because they suppress the body’s own defences. This can delay healing and promote an additional bacterial infection (then the doctor prescribes antibiotic eye drops).
In the case of an eye infection with herpes simplex viruses, under no circumstances should cortisone-containing eye drops be used, as this could aggravate the infection and lead to serious complications.
Treatment of allergic conjunctivitis (conjunctivitis allergic)
In the case of allergic conjunctivitis (conjunctivitis allergic), you should avoid the personal allergy trigger (allergen) if possible, e.g. pollen, cat dander or dust.
As with viral conjunctivitis, cold compresses and artificial tears can also reduce the symptoms of allergic conjunctivitis (conjunctivitis allergic)
Eye drops with antihistamines (anti-allergic active ingredients) serve the same purpose : Often, over-the-counter preparations can already achieve sufficient improvement. If not, the doctor can prescribe more powerful antihistamine eye drops. Alternatively or additionally, he can also prescribe eye drops with anti-inflammatory and pain-relieving NSAIDs (such as ketorolac) and/or mast cell stabilizers (such as azelastine). The latter, like antihistamines, have an antiallergic effect.
In persistent cases of allergic conjunctivitis (conjunctivitis allergic), short-term use of cortisone eye drops may be helpful. Before that, however, a herpes simplex infection of the eyes must be ruled out.
Depending on the type of allergy underlying the allergic conjunctivitis, causal treatment in the form of desensitization (hyposensitization) can be considered. The body slowly gets used to the disease-causing allergen. In the best-case scenario, the affected individual no longer reacts at all with hypersensitivity reactions such as allergic conjunctivitis (conjunctivitis allergic).
Other types of conjunctivitis: treatment
Whether foreign bodies, contact lenses or sun exposure are the causes of conjunctivitis – the therapy always consists of removing or avoiding the trigger. For example, foreign bodies or caustic substances in the eye are flushed out as quickly and completely as possible, contact lenses are removed, further UV radiation is avoided.
Depending on the cause, further treatment measures are useful. For example, in the case of conjunctivitis as a result of dry eyes, artificial tears (e.g. with hyaluronic acid) can alleviate the symptoms. They wet the eye and keep it moist. Eye drops with hyaluronic acid provide additional moisture because the substance binds water.
Home remedies for conjunctivitis
What to do with conjunctivitis, besides going to the doctor and, if necessary, using recommended medications? You can – preferably in consultation with your doctor – try home remedies to relieve the symptoms of conjunctivitis and support the healing process – regardless of the cause of the inflammation.
For example, you can put cool compresses on your closed eyes, such as a cold quark pad. It can help against itching and burning of the eyes and also has a decongestant and anti-inflammatory effect. Many people also use certain medicinal plants for an eye compress. Eyebright and calendula, for example, are valued for their anti-inflammatory properties.
Before using home remedies, you should first go to the eye doctor so that he can determine the cause and severity of the conjunctivitis and prescribe any necessary medication. Otherwise there is a risk of serious damage to the eye!
Home remedies have their limits. If the symptoms persist over a longer period of time, do not get better or even get worse, you should always consult a doctor.
Is conjunctivitis contagious?
Viral or bacterial conjunctivitis is very contagious. You can reduce the risk of infection with the following tips :
- Avoid rubbing your eyes : An inflamed conjunctiva is often itchy, tempting you to rub your eyes. Germs get on your hands and possibly in the other (still healthy) eye if you unconsciously reach out. Infected hands can also transmit the pathogens to doorknobs or cutlery, for example – a source of infection for other people. So try to resist the urge to rub.
- Washing hands : Frequent, correct hand washing and disinfecting hands reduce the number of germs on the fingers.
- Own towel : Use your own towel or, even better, disposable towels that you throw away immediately after use. This is how you protect other household members from contracting conjunctivitis.
- No handshakes : Even if it seems unfriendly – do not shake hands if you have conjunctivitis. Even if you avoid it, you often unknowingly touch your eyes, so that germs can quickly be transmitted via your hands.
- Don’t share eye drops : If you use eye drops (any kind) – don’t share them with other people.
Diagnosis of conjunctivitis
If you suspect conjunctivitis, you should always see an ophthalmologist! He will first collect your medical history in a personal conversation. He will ask you, for example, which complaints you have exactly, how long they have existed and whether you know the trigger. Information on possible underlying diseases such as diabetes or an allergy is also helpful for the doctor. This information can often be used to narrow down the possible causes of red eyes.
This is followed by eye examinations: Using a slit lamp examination, the doctor can examine the front area of the eye for signs of conjunctivitis (possibly involving the cornea = keratoconjunctivitis).
A careful folding of the eyelids can uncover inflammations – these leave typical traces on the inside of the eyelids. Any small foreign bodies that may be present in the eye can also often be discovered. This examination is seldom really uncomfortable for patients.
Depending on the suspected cause, further investigations may be necessary to clarify the problem. For example, the Schirmer test can help if wetting disorders are suspected. The tear secretion is determined with a filter paper strip in the conjunctival sac.
A swab from the conjunctiva can show whether and – if so – which pathogens are the reason for infectious conjunctivitis.
If there are signs of allergic conjunctivitis, an allergy test can determine the unknown trigger.
Conjunctivitis: course and prognosis
Infectious conjunctivitis usually heals without consequences – and often no medication is required. With some infections – especially those with certain bacteria – the inflammation can last for a long time (possibly become chronic) or cause complications if left untreated.
Chlamydia conjunctivitis, for example, can progress as so-called trachoma, especially under poor hygienic conditions, and then under certain circumstances lead to progressive scarring of the conjunctiva. This can limit vision and even lead to blindness! In fact, trachoma is the leading cause of acquired blindness worldwide.
Early treatment is also very important for gonococcal conjunctivitis. Otherwise, if the cornea is involved, there is a risk of reduced vision and even blindness.
Conjunctivitis in newborn children can also result in blindness, so it should be treated promptly and properly.
In the case of non-infectious conjunctivitis, the prognosis depends largely on whether and how well the trigger can be eliminated or avoided (e.g. in the case of allergic or foreign body-related conjunctivitis). If conjunctivitis occurs as a result of an injury (such as a burn or chemical burn), the severity of the eye damage also plays a role.