What is the dermatomyositis juvenile?
Dermatomyositis Juvenile is a rare disease that affects the muscles and skin. The disease is defined as “juvenile” when it develops before the age of 16 years.
Dermatomyositis Juvenile belongs to a group of pathological conditions that are considered autoimmune diseases. Normally, the immune system helps us fight infections. In autoimmune diseases, the immune system reacts differently: it becomes overactive in normal tissue. This reaction of the immune system leads to inflammation, which causes swelling of the tissue and can lead to tissue damage.
Dermatomyositis Juvenile affects small blood vessels in the skin (dermato-) and muscles (myositis). This leads to problems such as muscle weakness or pain, especially in the muscles of the trunk, but also in the muscles of the hips, shoulders and neck. Most patients also have typical skin rashes. These rashes can appear on several areas of the body: on the face, eyelids, fingers, knees and elbows. The onset of a skin rash does not always coincide with muscle weakness: the rash may develop before or after the onset of muscle weakness. In rare cases, small blood vessels in other organs may also be affected.
Dermatomyositis can develop in children, adolescents, and adults. Dermatomyositis Juvenile has a number of differences from adult dermatomyositis. Approximately 30% of adults with dermatomyositis have an association between the disease and cancer, while in dermatomyositis juvenile there is no association with cancer.
How common is this condition?
Dermatomyositis Juvenile is a rare disease in children. Every year, Dermatomyositis Juvenile develops in approximately 4 children per million. The disease is more common in girls than boys. It most often begins between the ages of 4 and 10, but can develop in children of any age. dermatomyositis juvenile can develop in children regardless of where they live or their ethnicity.
Causes of dermatomyositis juvenile
The exact cause of dermatomyositis is unknown. There is a lot of research going on around the world to find out what causes Dermatomyositis Juvenile.
Dermatomyositis Juvenile is now thought to be an autoimmune disease and is most likely caused by a combination of factors. These may include a person’s genetic predisposition combined with exposure to environmental triggers such as ultraviolet radiation or infections. Studies have shown that some microorganisms (viruses and bacteria) can cause a malfunction in the immune system. Some families with children with Dermatomyositis Juvenile also have other autoimmune diseases (diabetes mellitus or arthritis, for example). However, there is no increased risk that Dermatomyositis Juvenile will develop in a second family member.
There is currently nothing we can do to prevent the development of Dermatomyositis Juvenile. Most importantly, there was nothing you could do as a parent to prevent your child from getting Dermatomyositis Juvenile.
Is this disease infectious?
Dermatomyositis Juvenile is not an infectious disease, it is not contagious.
Symptoms of dermatomyositis juvenile?
Different patients have different symptoms of dermatomyositis juvenile. Most children experience:
Fatigue
Children are often tired. This can lead to limited exercise capacity and ultimately potentially cause difficulty in daily activities.
Muscle pain and weakness
The disease often affects the muscles in the trunk, as well as the muscles of the abdomen, back and neck. From a practical point of view, the child may begin to refuse long walks and sports, small children may “become capricious”, asking to be held. As dermatomyositis juvenile symptoms worsen, climbing stairs and getting out of bed can become a problem. In some children, inflamed muscles become stiff and contract (called contractures). This makes it difficult for the child to fully straighten the affected arm or leg: the elbows and knees are usually in a fixed flexed position. This can affect the range of motion of the arms or legs.
Joint pain and sometimes swelling and stiffness
With dermatomyositis juvenile both large and small joints can become inflamed. This inflammation can cause the joint to swell, as well as cause pain and make it difficult to move the joint. Inflammation responds well to treatment and usually does not lead to joint damage.
Skin rashes
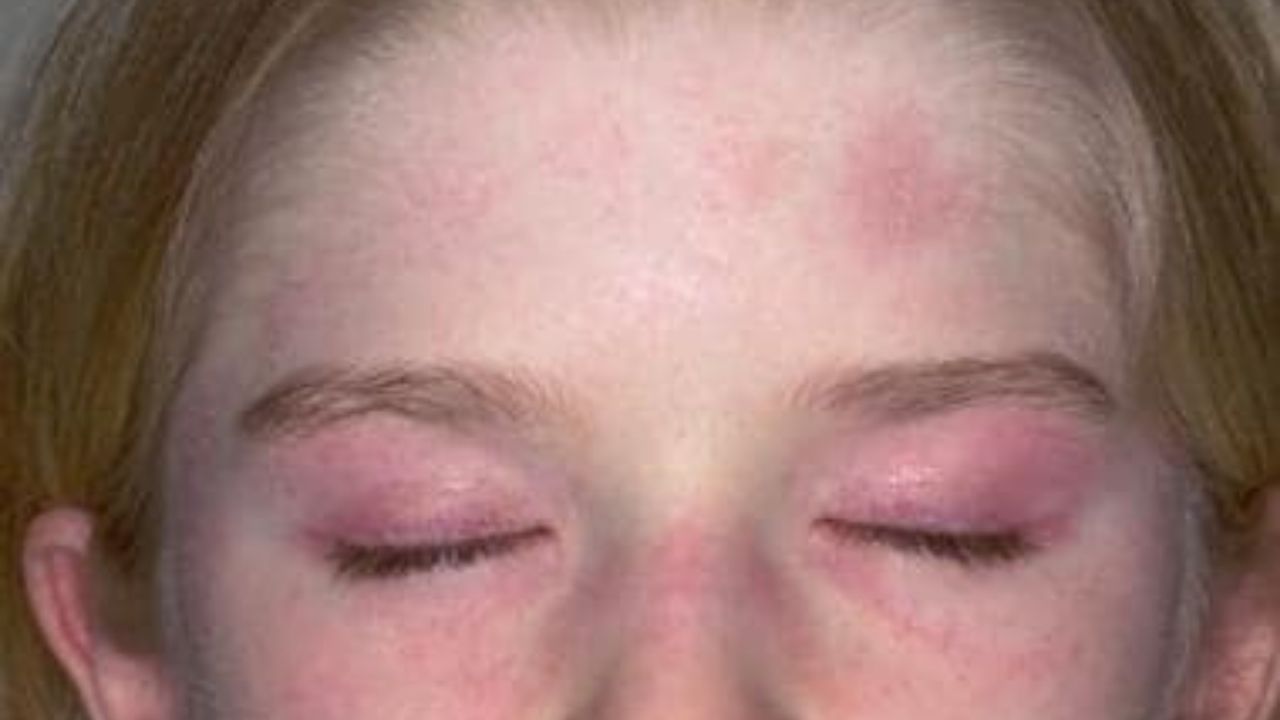
The rash typical of dermatomyositis juvenile may be on the face, be accompanied by swelling around the eyes (periorbital oedema), appear as purplish-pink spots on the eyelids (a symptom of “purple glasses”), on, and also on other parts of the body (in the upper part of the knuckles, on knees and elbows) where the skin may thicken (Gottron’s papules). Skin rashes can develop long before muscle pain or weakness appears. In children with dermatomyositis juvenile, the rash may also appear on other parts of the body. Sometimes doctors may see swollen blood vessels (appearing as red dots) in the child’s nails or eyelids. In some cases, a dermatomyositis juvenile rash is sensitive to sunlight (photosensitivity), while in other cases it can lead to ulcers.
Calcinosis
In the course of the disease, indurations under the skin containing calcium may develop. This is called calcification. Sometimes it is present at the very beginning of the disease. Ulcers may appear on the surface of such hardenings, from which a milky liquid containing calcium may ooze. Ulcers are difficult to treat.
Abdominal pain
Some children have bowel problems. These problems include abdominal pain or constipation, and sometimes serious problems in the abdominal cavity – this is due to damage to the blood vessels of the intestine.
Lung injury
Breathing problems can occur due to muscle weakness. In addition, muscle weakness can cause changes in the child’s voice, as well as difficulty swallowing. In some cases, pneumonia develops, which can lead to shortness of breath.
In the most severe cases, the disease affects virtually every muscle that attaches to the skeleton (skeletal muscle), resulting in problems with breathing, swallowing, and speaking. In this regard, important signs of the disease are a change in voice, difficulty feeding or swallowing, coughing and shortness of breath.
Do all children experience the same disease?
The severity of the disease is different for each child. In some children, the disease affects only the skin without any muscle weakness (dermatomyositis without myositis), or with very mild muscle weakness that can only be detected by testing. In other children, the disease can affect many parts of the body: the skin, muscles, joints, lungs, and intestines.
Is the disease different in children than in adults?
In adults, dermatomyositis may be secondary to cancer (malignant neoplasms). In dermatomyositis juvenile, the association with cancer is extremely rare.
In adults, a disease develops in which only the muscles (polymyositis) are affected, in children this pathology is very rare. Adults sometimes develop specific antibodies that are found on examination. In children, most antibodies are not detected, but over the past 5 years, the presence of specific antibodies in children has been shown. Calcification is more common in children than in adults.
How is dermatomyositis juvenile diagnosed?
To diagnose dermatomyositis juvenile, a child will need a physical examination, along with blood tests and other tests such as an MRI or muscle biopsy. Every child is different and your doctor will decide which tests and examinations are best for the child. Dermatomyositis Juvenile may present with a distinct pattern of muscle weakness (the disease affects the muscles of the hips and shoulders) and specific skin rashes: in these cases, Dermatomyositis Juvenile is easier to diagnose. A physical examination will include an assessment of muscle strength, examination of the skin and nail plates for rashes and vascular lesions.
Occasionally, Dermatomyositis Juvenile may resemble other autoimmune diseases (such as arthritis, systemic lupus erythematosus, or vasculitis) or congenital muscle diseases. The tests will help you find out what disease your child has.
Blood tests
Blood tests are done to check for inflammation, immune system function, and problems that are identified as a result of inflammation, such as “leaky” muscles. In most children with dermatomyositis juvenile, the muscles become “leaky”. This means that some of the substances contained in muscle cells enter the bloodstream, where their content can be measured. The most important of these are proteins called muscle enzymes. Blood tests are commonly used to determine how active the disease is and to assess response to treatment during follow-up (see below). There are five muscle enzymes that can be measured in the blood: CK (creatine kinase), LDH (lactate dehydrogenase), AST (aspartate aminotransferase), ALT (alanine aminotransferase), and aldolase. Level, at least one of these proteins is elevated in most patients, although not always. There are other laboratory tests that can help in the diagnosis. We are talking about analyzes that determine the content of antinuclear antibodies (ANA), myositis-specific antibodies (MSA) and myositis-associated antibodies (MAA). Analysis for ANA and MAA can be positive in other autoimmune diseases.
MRI
Muscle inflammation can be seen using magnetic resonance imaging (MRI) techniques.
Other methods of muscle examination
The results of a muscle biopsy (removal of small pieces of muscle) are important in confirming the diagnosis. In addition, a biopsy can be a tool for scientific research aimed at deepening the understanding of the causes of this disease.
Functional changes in the muscle can be measured using special electrodes that are inserted like needles into the muscles (electromyography, EMG). This study allows a distinction between dermatomyositis juvenile and some congenital muscle diseases, but in simple cases this is not necessary.
Other examinations
Other examinations may be performed to detect damage to internal organs. Electrocardiography (ECG) and cardiac ultrasound (ECHO) can detect heart involvement, and chest x-ray or computed tomography (CT), along with lung function tests, can detect lung involvement. X-ray of the swallowing process using a special opaque liquid (contrast agent) allows you to find out if the muscles of the pharynx and esophagus are involved. Abdominal ultrasound is used to assess the condition of the bowel.
What is the meaning of tests?
Typical cases of dermatomyositis juvenile can be diagnosed based on the pattern of muscle weakness (muscle involvement in the hips and shoulders) and the classic skin rash. Tests and examinations are then used to confirm the diagnosis of dermatomyositis juvenile and monitor treatment. Muscle status in dermatomyositis juvenile can be assessed using standardized measures of muscle strength (Children’s Myositis Rating Scale (CMDS), Manual Muscle Testing 8 (MMT8)) and blood tests (to detect elevated muscle enzyme levels and indicators of inflammation).
Treatment of dermatomyositis juvenile
Dermatomyositis Juvenile is a treatable disease. There is no cure for this disease, but the goal of treatment is to bring the disease under control (go into remission). Treatment is tailored to the needs of each individual child. If the disease is not controlled, then damage to various organs is possible, and this damage can be irreversible: this can lead to long-term problems, including disability, which persists even when the disease passes.
For many children, physiotherapy is an important element of treatment; some children and their families need psychological support to cope with illness and its impact on their daily lives.
What are the treatments?
All drugs used to treat dermatomyositis juvenile suppress the immune system to stop inflammation and prevent organ damage. Corticosteroids These drugs are great for quickly relieving inflammation. Sometimes corticosteroids are given by vein (by intravenous injection or drip) to help the body get the medicine quickly. In some cases, this saves a person’s l
However, if high doses need to be administered for a long time, side effects are possible. Side effects of corticosteroids include growth retardation, increased risk of infection, high blood pressure, and osteoporosis (thinning of the bone). Corticosteroids cause some problems at low doses, but most problems occur at higher doses. Corticosteroids inhibit the body’s production of its own steroids (cortisol), and if the drug is suddenly stopped, it can lead to serious problems, sometimes even life threatening. That is why the dose of corticosteroids must be reduced gradually. Other immunosuppressive drugs (such as methotrexate) may be given along with corticosteroids for long-term control of inflammation.
Methotrexate
With its use, the effect is noted after 6-8 weeks, and it is usually applied over a long period. Its main side effect is nausea associated with the administration of the drug. Occasionally, mouth ulcers, mild thinning of hair, a decrease in white blood cells in the blood, or an increase in liver enzymes may occur. Liver problems are usually minor, but they can be greatly exacerbated if the patient drinks alcohol. The addition of a vitamin called folate or folinic acid reduces the risk of side effects, especially those associated with impaired liver function. There is a theoretical possibility of an increased risk of infections, although in practice this kind of problem has not been noted, with the exception of chickenpox. During treatment, pregnancy should be avoided,
If the disease is not controlled with a combination of corticosteroids and methotrexate, a number of other treatments may be used; they are often given as a combination treatment.
Other immunosuppressants
• Cyclosporine, like methotrexate, is usually used for a long time. Its long-term side effects include increased blood pressure, increased body hair growth, swollen gums, and kidney problems.
• Mycophenolate mofetil has also been used for a long time. This drug is generally well tolerated. The main side effects include abdominal pain, diarrhea and an increased risk of infections.
• Cyclophosphamide may be given in severe cases or when the disease does not respond to other means.
Intravenous immunoglobulin (IVIG)
This medicine contains concentrated antibodies isolated from human blood. It is injected into a vein and has worked well for some patients by acting on the immune system and reducing inflammation. The exact mechanism of action of this drug has not been studied.
Therapeutic exercise and exercise
The typical physical symptoms of dermatomyositis juvenile are muscle weakness and joint stiffness, which leads to decreased mobility and poor fitness. Contraction of affected muscles can lead to limited ability to move. These problems can be overcome by conducting regular sessions of physiotherapy exercises. The physical therapy specialist will teach children and their parents how to do stretching, strengthening and fitness exercises. The goal of treatment is to increase muscle strength and endurance, and to improve and maintain joint range of motion. It is extremely important that parents are involved in this process and can help the child adhere to the exercise program.
Treatment with ancillary drugs
Proper intake of calcium and vitamin D is recommended.
How long should treatment last?
The duration of treatment for each child is different. It will depend on how dermatomyositis juvenile affects the child. Most children with dermatomyositis juvenile are treated for at least 1-2 years, but some children need treatment for many years. The goal of treatment is to control the disease. The intensity of treatment can be gradually reduced, and once dermatomyositis juvenile has become inactive for a certain time (usually for many months), treatment can be stopped. Inactive dermatomyositis juvenile is defined in a child who feels well, has no signs of active disease, and his blood tests are normal. Assessment of inactive disease is a thorough process in which all aspects must be considered.
Can non-traditional therapies / complementary therapies be used?
There are many complementary and alternative treatments available and this can be confusing for patients and their families. Most treatments have not been proven effective. Carefully weigh the risks and benefits of these therapies, as they are not proven to be effective and can be costly in terms of money, time, and burden on the child. If you wish to explore complementary and alternative treatments, it makes sense to discuss these options with your pediatric rheumatologist. Some treatments may interact with conventional medications. Most doctors won’t mind complementary treatments, as long as you follow your doctor’s recommendations. It is very important not to stop taking the medicines prescribed by your doctor. When drugs such as corticosteroids are needed to control JDM, stopping them while the disease is still active can be very dangerous. Please discuss your drug concerns with your child’s doctor.
Medical examinations
Regular medical checkups are very important. During these activities, dermatomyositis juvenile activity and potential side effects of treatment will be monitored. Because many parts of the body can be affected in dermatomyositis juvenile, the doctor needs to carefully examine the entire child. Sometimes special tests are performed to measure muscle strength. A blood test is often required to check disease activity and monitor the effectiveness of treatment.
Prognosis of dermatomyositis juvenile
As a rule, dermatomyositis juvenile takes place in the following 3 forms:
Dermatomyositis juvenile with monocyclic course: only one episode of disease that goes into remission (i.e., inactive disease) within 2 years after the onset of the disease, without relapse;
Dermatomyositis juvenile with polycyclic course: there may be long periods of remission (the disease is inactive and the child feels well) alternating with periods of relapse of dermatomyositis juvenile, which often occur if treatment is reduced or stopped;
Chronically active disease: persistently active dermatomyositis juvenile despite treatment (chronic relapsing-remitting disease); this latter group has a higher risk of developing complications.
Compared to adults with dermatomyositis, children tend to feel better and do not develop cancer (malignant growths). In children in whom dermatomyositis juvenile affects internal organs such as the lungs, heart, nervous system, or intestines, the disease is much more severe. dermatomyositis juvenile can be life-threatening, but it depends on how severe the disease is, including the severity of muscle inflammation, which organs are affected, and whether there is calcification (lumps of calcium under the skin). Long-term problems can be caused by muscle tension (contractures), muscle loss, and calcification.
DAILY LIFE
How can the illness affect my child and my family’s daily life?
Attention should be paid to the psychological impact of the disease on children and their families. Chronic diseases, such as dermatomyositis juvenile, cause difficulties for the whole family and, of course, the more serious the form, the more difficult it is to cope with the disease. It will be difficult for a child to properly cope with the disease if his parents have problems with this. It is extremely important to have a positive attitude on the part of the parents and encourage the child to strive for independence, if possible, despite the illness. This helps children to overcome the difficulties associated with the disease, to succeed in school on an equal basis with their peers, and to be independent and balanced. If needed, the pediatric rheumatologist should offer psychological support.
One of the main goals of therapy is to enable the child to lead a normal life as an adult. In most cases, this is successful. . The treatment of dermatomyositis juvenile has improved significantly over the past ten years, and it is safe to say that several new drugs will appear in the near future. Currently, the combined use of pharmacological treatment and rehabilitation is able to prevent or limit muscle damage in most patients.
Can exercise and exercise therapy help my child?
The goal of exercise and exercise therapy is to help the child participate as fully as possible in all normal daily activities and to fulfill his or her potential in society. Physical exercise and exercise therapy can also be used to encourage an active healthy lifestyle. In order to achieve these goals, you need healthy muscles. Exercise and exercise therapy can be used to improve muscle flexibility, muscle strength, coordination and endurance (increased vitality). These aspects of musculoskeletal health will enable children to successfully and safely participate in school activities as well as extracurricular activities such as leisure activities and sports. Treatment and a set of exercises performed at home,
Can my child play sports?
Sports are an important aspect of every child’s daily life. One of the main goals of exercise therapy is to ensure that such children are able to lead a normal life and not see themselves as different from their friends. The general advice is for patients to play the sports they want to do, but to explain to them the need to stop when muscle pain occurs. This will allow the child to start playing sports at an early stage of treatment of the disease; partial restriction of sports is better than a complete rejection of exercise and sports with friends due to illness. The general attitude should encourage the child to be independent within the limits of the disease. Before starting exercise, it is necessary to consult with a specialist in physiotherapy exercises (and sometimes they need to be carried out under the supervision of such a specialist). The physical therapy specialist will tell you which exercises or sports are safe for the child, as this will depend on how weak the child’s muscles are. The load should increase gradually to strengthen the muscles and improve endurance.
Can my child attend school regularly?
School for children is no less important than work for adults: it is a place where children learn to become an independent and self-reliant person. Parents and teachers should provide flexibility so that children can participate as normally as possible in school activities. This will help the child to be the most successful in school, as well as to integrate and be accepted by both peers and adults. It is extremely important that children attend school regularly. There are several factors that can cause problems: difficulty walking, fatigue, pain, or stiffness. It is important to explain to teachers what the needs of the child are. He needs: help with writing difficulties, an appropriate desk for work, being able to move regularly to avoid muscle stiffness, and facilitating participation in some physical education activities. Patients should be encouraged to actively participate in physical education classes whenever possible.
Can diet help my child?
There is no evidence that diet can influence the disease process, but a normal balanced diet is recommended. A healthy, well-balanced diet rich in protein, calcium and vitamins is recommended for all growing children. Patients taking corticosteroids should avoid overeating, as these drugs cause increased appetite, which can easily lead to excessive weight gain.
Can climate affect my child’s illness?
The relationship between ultraviolet radiation and dermatomyositis juvenile is currently being studied.
Can my child be vaccinated or have vaccinations?
Immunizations should be discussed with your doctor, who will decide which vaccines are safe and appropriate for your child. Many vaccinations are recommended: tetanus, polio by injection, diphtheria, pneumococcal and influenza by injection. These vaccinations are performed using non-live compound vaccines that are safe for patients taking immunosuppressive drugs. However, vaccinations using live attenuated vaccines should generally be avoided. This is due to the hypothetical risk of infection induction in patients receiving high doses of immunosuppressive or biological drugs (for example, vaccinations against mumps, measles, rubella, BCG, yellow fever).
Are there problems with sexuality, pregnancy or contraception?
There is no evidence that dermatomyositis juvenile affects sexual activity or pregnancy. However, many of the drugs used to fight this disease can have adverse effects on the fetus. Sexually active patients are advised to use safe contraceptives and to discuss contraception and pregnancy with their doctor (especially before preparing to conceive a child).
